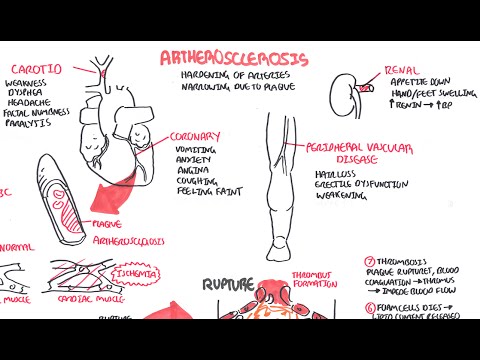
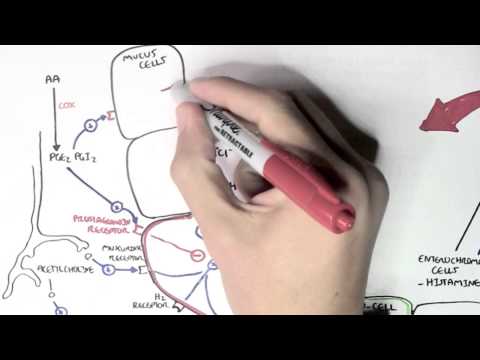
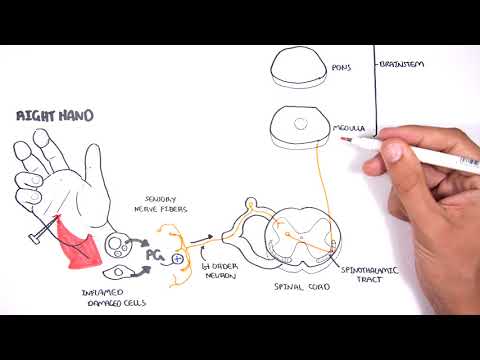
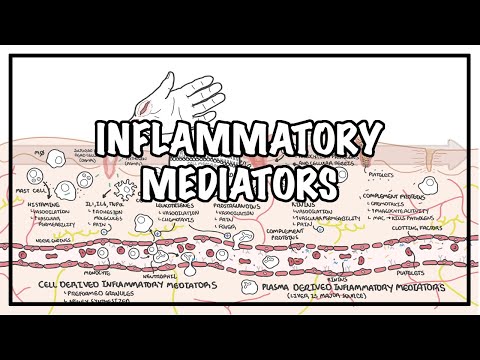
0:00 There are many factors which influence or stimulate tissue repair. 0:14 The cytokines, for example, stimulate fibroblasts to proliferate, and also to 0:19 increase their 0:20 collagen synthesis. 0:23 This mechanism stimulates or causes repair of tissues. 0:28 If there are damaged blood vessels, coagulation cascade is performed, which 0:33 repairs damaged 0:34 blood vessels, chemotaxis also promotes tissue repair. 0:40 Now going back into the inflammatory mediators, remember we had two types, the 0:44 plasma derived 0:45 and the cell derived. 0:47 The cell derived are the cytokines, for example, and also histamine, for 0:52 example. 0:53 These are cell derived because they come from cells, they are made from cells. 0:59 Okay, so anyway, all these inflammatory mediators promote the recruitment of 1:05 immune cells such 1:07 as macrophages and neutrophils from the blood vessel into the tissue. 1:12 These neutrophils and macrophages express special receptors for PAMP, as I 1:18 mentioned. 1:20 So now, for example, this neutrophil binds onto these pathogens with this 1:23 receptor and 1:24 can engulf it. 1:26 So how about the complement proteins, the plasma inflammatory mediator, what do 1:31 they do? 1:33 Well, if a bacteria or the pathogen is present, the complement protein with 1:40 antibodies can 1:41 cause few things to happen. 1:44 It can cause obstinization or it can essentially create a hole within the path 1:52 ogen, causing 1:54 it to lice. 1:56 So let's talk about obstinization first. 1:58 Obstinization of pathogens by complement proteins and antibodies essentially 2:02 coats the pathogen. 2:03 What this allows for phagocytes such as neutrophils and macrophages to detect 2:09 these pathogens more 2:10 easily, to destroy it. 2:14 Now, lysis of pathogen is essentially when a hole is created on the pathogen, 2:20 the bacteria, 2:21 causing it to burst. 2:25 Complement proteins such as C3A and C5A are very important inflammatory medi 2:32 ators as well 2:33 as they promote inflammation. 2:36 They work as a chemoattractant to attract more immune cells and they also 2:40 increase vascular 2:42 permeability, allowing more recruitment of immune cells. 2:49 These complement proteins, the C3A and C5A, because it's a chemoattractant, it 2:55 also stimulates 2:56 the repair of tissues as well. 3:00 So as you can see, the complement proteins are important in the innate immune 3:04 response, 3:05 in the inflammatory response. 3:07 Let's look at some other inflammatory mediators, but now instead of looking at 3:12 the plasma, 3:13 let's look at the cell-derived inflammatory mediators. 3:15 Remember, they were cytokines and they were histamine. 3:20 Other inflammatory mediators coming from the cells are the arachidonic acid 3:28 metabolites. 3:29 So for example, endothelial cells, mast cells, as well as other types of immune 3:34 cells, particularly 3:35 the granular sites, can secrete prostaglandins, which is an arachidonic acid 3:42 metabolite. 3:43 Prostaglandins induce fever and also cause pain. 3:49 Mast cells, again, as well as other types of cells, such as basophils, can sec 3:55 rete also 3:56 leukotrienes, and these are also arachidonic acid metabolites. 4:02 They work as a chemoattractant and also increase vascular permeability, and 4:08 therefore they 4:08 promote inflammation. 4:11 So these arachidonic metabolites, the leukotrienes and prostaglandins, are 4:16 inflammatory mediators, 4:19 cell-derived inflammatory mediators. 4:22 So essentially from this whole map, all these inflammatory mediators and 4:26 everything, the 4:27 histamine, cytokines, common proteins, et cetera, et cetera, they cause the 4:33 characteristics 4:34 of inflammation. 4:37 And there are four Greek words, as well as just an English word, that denotes 4:41 the characteristics 4:42 of inflammation. 4:45 The first two are rubor and calor, which denotes redness and heat. 4:52 And this is due to the dilating blood vessels. 4:56 Then we have two more, which is swelling. 4:58 And this is due to the leakage of plasma fluids and also the proteins from the 5:02 blood 5:03 vessels into the tissue. 5:07 The fourth Greek word that denotes inflammation is dolar, which is also Latin, 5:11 I think, and 5:12 that denotes pain. 5:13 And this is due to the sensory nerve fibers firing, and also it can be 5:17 mechanical damage 5:19 to the nerves, and also prostaglandins, remember, causes pain. 5:25 Now, there can also be a fifth characteristic of inflammation, which is loss of 5:29 function, 5:29 and this is usually when it's chronic inflammation. 5:38 Now as we know, the immune cells play a critical role in their inflammatory 5:42 response. 5:43 What just happened with all these inflammatory mediators are part of the innate 5:48 immune system. 5:49 But if a pathogen causes an infection in the body, the adaptive immune system 5:54 has to 5:54 be initiated. 5:56 These are the cells within the lymph nodes. 5:59 So what can happen is, antigen-presenting cells, such as dendritic cells or mac 6:04 rophages, 6:05 can engulf the bacteria or the pathogen. 6:08 This will activate the antigen-presenting cell, which will then allow them to 6:14 travel 6:15 to the lymph node via the lymph vessel and to activate the adaptive immune 6:19 response, to 6:20 activate the cells within the lymph node, the naive B and T cells. 6:25 So here, this dendritic cell, upon activation, travels to the lymph node with 6:31 the antigen 6:32 of the pathogen, essentially with the pathogen. 6:35 And with the pathogen, it will activate the naive B cell and T cell. 6:39 The naive B cell will become a plasma cell, which can secrete antibodies. 6:45 And the naive T cell will become either a T helper cell or a T killer cell. 6:51 These cells are the lymphocytes, and they are part of the adaptive immune 6:55 response. 6:56 They are very specific and will attack the pathogens that has invaded the body 7:02 specifically. 7:04 So for example, we won't really talk about them, but the plasma cells will sec 7:09 rete antibodies, 7:10 such as IgM, IgG and IgD, and these antibodies will stimulate the inflammatory 7:16 response and 7:17 try to remove the pathogens and bring the body back to normal state. 7:23 If you want to learn more about the adaptive immune response and the innate 7:26 immune response 7:27 specifically, I've got a video on that, and I'll provide the link at the end of 7:31 this video. 7:32 So that is it for inflammation. 7:35 I hope you understood it. 7:39 As you can see, there are many factors playing a role in the inflammatory 7:44 process, in the 7:45 inflammatory response, particularly the inflammatory mediators. 7:50 Thank you for watching.