Petechial, Purpuric Rash
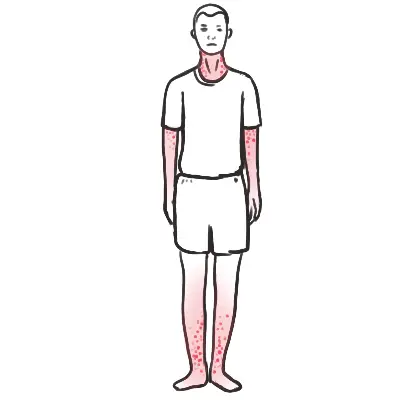

At least 90% of children with fever and petechiae will NOT have meningococcal disease. However, recognition and early treatment of the child with meningococcal disease is paramount. All children with fever and petechiae should be reviewed by a registrar or consultant. If invasive meningococcal disease is suspected, administer parenteral antibiotics immediately, but do not delay hospital admission.
| Remember A cardinal sign of a purpuric rash is that it does not blanch on pressure, unlike exanthema, telangiectases, or allergic rashes. |
| Definitions Petechiae: Pinpoint non-blanching spots. Purpura: Larger non-blanching spots (>2mm) |
| Remember The majority of children with fever and petechiae do not have a cause identified – they are presumably due to viral infections. |
Purpuric rash + Normal thrombocyte levels (Thrombocytopenic purpuric syndromes)
| Henoch Schonlein pupura triad: Abdominal pain, rash starting from lower limb and moving up, arthlagia. |
Purpuric rash + Thrombocytopaenia
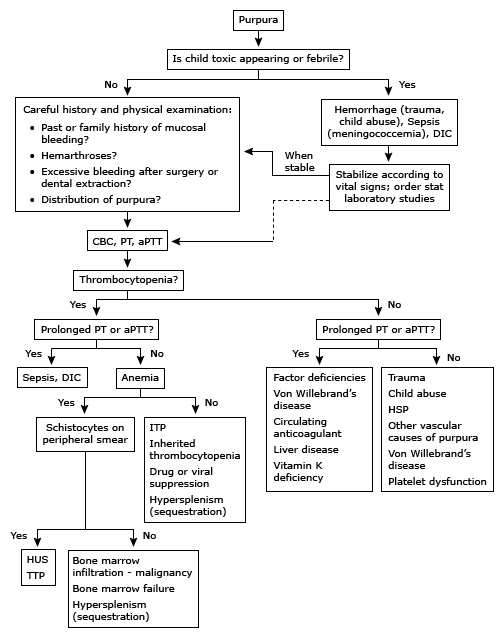

Discussion