Overview
Osteoarthritis (OA) was previously thought to be a normal consequence of aging, leading to the term “degenerative joint disease.” However, it is now realized that osteoarthritis results from the interplay of multiple factors, including joint integrity, genetics, local inflammation, mechanical forces, and cellular and biochemical processes. Pathological changes include joint space narrowing, damage of articular cartilage, subchondral sclerosis and bone spurs/cysts.
| Definition Arthritis: Inflammation of a/multiple joints Arthropathy: Joint pathology, any disease of the joint Arthrosis: a term for a degenerative disease of the joint where the cartilage lining the joint erodes over time. Usually used for osteoarthritis. Osteoarthritis: is a degenerative condition that mostly affects the hands, spine and joints such as hips, knees and ankles, and usually gets worse over time. Rheumatoid arthritis: a chronic progressive disease causing inflammation in the joints and resulting in painful deformity and immobility, especially in the fingers, wrists, feet, and ankles. |
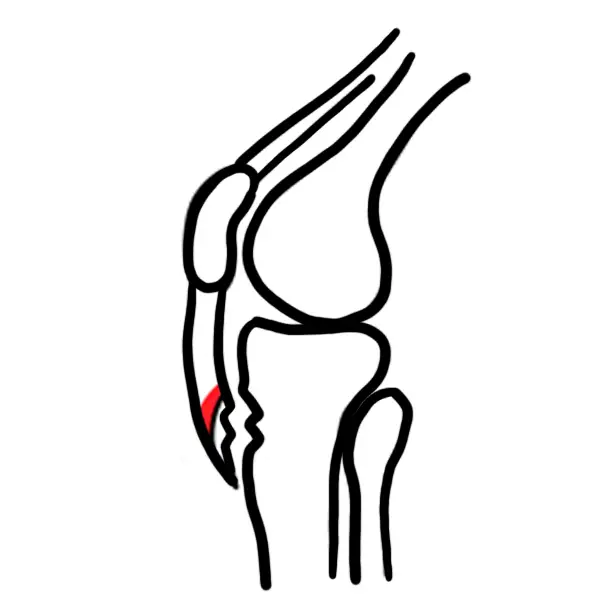
Anatomy
The knee joint is a synovial joint, in that it is encapsulated by the synovial membrane which produced synovial fluid. As the knee is a modified hinge joint it is structured to perform two principal actions, flexion (bending) and extension (straightening). The muscles which act at the knee are predominantly the quadriceps (extension) and the hamstrings (flexion). The knee can also do a bit of internal and external rotation.
The knee joint is made up of three main bones:
- Patella
- Femur
- Tibia
Cartilage The ends of the bones are covered by articular cartilage. Between these bone articulation there is also the meniscus, another type of cartilage. The menisci are C-shaped fibrocartilaginous disks in the knee (lateral more O-shaped).
Risk Factors
Mainly age >50, female, genetics and previous knee injuries. Obesity and knee malignment accelerates the development of osteoarthritis.
Signs and Symptoms
Most commonly presents in patients over 40 years of age
- Pain
- Exacerbated by activity and relieved by rest
- Severe, pain occurs at rest and at night
- Weather can affect pain
- Stiffness
Clinical Examination
- Tenderness to palpation of involved joints may be evident with or, more often, without associated signs of inflammation.
- Joint effusions may be present, which typically exhibit a mild pleocytosis, normal viscosity, and modestly elevated protein.
- Crepitus is a common finding and is probably due to the disruption of the normally smooth articulating surfaces of the joints.
- Osteophytes may be palpable as bony enlargements along the periphery of the joint.
Differential Diagnosis
- Rheumatoid arthritis
- Crystal arthritis
- Meniscal injury
- Bursitis
| Remember Septic arthritis is not really a differential of osteoarthritis, but should be ruled out with any monoarthritic presentation. |
Investigations
- X-ray – Radiological findings: LOSS
- Loss of joint space
- Osteophytes
- Subchondral cysts
- Subchondral sclerosis
- MRI – if suspect associated soft tissue injury
- Inflammatory markers: ESR, CRP
- FBC
Advanced Investigations to rule out differentials
- Joint aspiration – crystal, septic
- Rheumatoid Factor antibody, Anti-CCP
- ANA
| Synovial fluid analysis | |||
| Aetiology | Colour and Clarity | WBC (mm³) | |
| Normal | Normal | Clear and transparent | <200 |
| Non-Inflammatory | Osteoarthritis | Yellow and transparent | 0 to 2000 |
| Inflammatory | Gout | Yellow and traslucent-opaque | 2000-100,000 |
| Septic | Bacteria | Yellow/green and opaque | >25,000 – >100,000 |
| Haemorrhage | Trauma | Red and Bloody | 200-2000 |
Pathophysiology
Management
Acute exacerbation
- Corticosteroid Injection
Ongoing/Long-term
- Non-pharmacological
- Pharmacological
- Surgical
| Remember The psychosocial evaluation should include an assessment of coping mechanisms, such as activity avoidance and denial, and of symptoms of depression. |
| Remember Gastroprotection with PPI if on long term NSAIDs. |
| Pharmacology NSAIDs inhibit COX1/COX2, enzymes responsible for converting arachidonic acid to Prostagladins, ThromoxaneA2. Prostaglandins promote inflammation, fever and pain. Thromboxane A2 causes platelet aggregation (blood clotting). Side effects: Increased BP, Dyspepsia, Peptic ulcer, duodenal ulcer, liver damage (rare and long-term), acute kidney injury, tinnitus (high-dose) and allergy. Contraindications: Pre-existing renal dysfunction, cardiac failure, severe hepatic dysfunction, history of GI bleeding, allergy, elderly >65. |
Surgical Treatment
- Arthroscopic washouts – with trimming of meniscal fragments and osteophytes, may give temporary relief
- Realignment osteotomy (typically an upper tibial valgus osteotomy for medial compartment disease in a young patient) is often successful in relieving symptoms and staving off the need for ‘end-stage’ surgery.
- Replacement arthroplasty is indicated in older patients with progressive joint destruction.
| Indications for Knee Replacement |
| Pain |
| Conservative treatment has failed |
Complications and Prognosis
Complications
- Septic arthritis from surgery
- Gastrointestinal bleeding from oral NSAID use
- Depression
Complications with Joint Replacement Surgery
- Infection
- Blood clots
- Loosening of the prosthesis
- Dislocation
- Nerve or blood vessel injury near prosthesis
- Problems with anaesthesia
- Wound irritation or breakdown
- Wear of joint
Prognosis Knee replacement is inevitable with patients with painful osteoarthritis. Knee replacements can last from 5-20 years depending on the activity level of the patient.




Discussion