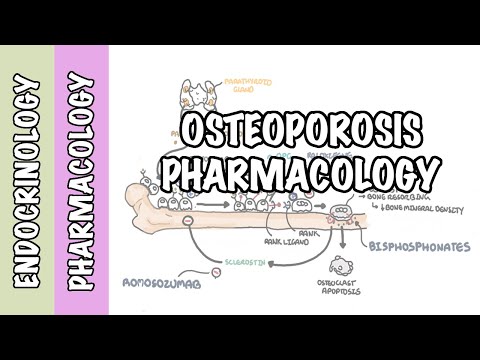
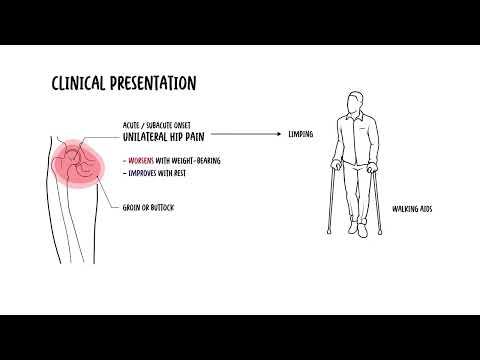
0:00 Glucocorticoids are used in many inflammatory and autoimmune conditions. 0:19 While being used to treat an underlying disease, glucocorticoids is associated 0:24 with an appreciative 0:26 risk of bone loss and increases the risk of fractures, which is actually more 0:32 pronounced 0:33 in the first few months of use. 0:37 In general, risk of glucocorticoid-associated osteoporosis and fractures 0:42 increases with 0:43 age, dose, and duration. 0:46 However, risk of fracture with glucocorticoids increases with doses as low as 2 0:53 .5 to 7.5 0:55 milligrams daily. 0:58 Glucocorticoids exerts their effects on gene expression via cytoplasmic glucoc 1:03 orticoid 1:04 type 2 receptors, binding of glucocorticoids to its receptor stimulates gene 1:10 expression, 1:11 which will ultimately cause the effects of the glucocorticoids on the body. 1:18 So specifically related to bones, glucocorticoids receptors are found in all 1:23 bone cells except 1:24 for osteoclasts. 1:28 Glucocorticoid use causes a negative feedback effect on the hypothalamus and 1:33 the pituitary 1:33 gland. 1:35 It actually acts as an exogenous cortisol essentially, so elevated glucocortic 1:40 oid levels will reduce 1:42 secretion of ACTH at an no-chorticotropic hormone, and also reduce the 1:49 secretion and 1:51 production of follicle-stimulating hormone, FSH, and luteinizing hormone, LH. 1:59 Reduction in ACTH results in reduced endogenous steroid hormone production from 2:04 the adrenal 2:05 glands, including cortisol and androgens. 2:09 Low FSH and LH reduces production of androgens and estrogens from the gonads. 2:16 Low androgens and estrogens increases the risk of osteoporosis, which will soon 2:21 see 2:21 why. 2:24 Your bones contain three main type of cells. 2:27 Your osteocytes, which will essentially become osteoblasts, you have your oste 2:32 oblasts, 2:32 the bone-building cells, and osteoclasts, and in this case, immature osteocl 2:37 asts, 2:38 termed pre-osteoclasts. 2:41 Glucocorticoids stimulate osteocyte apoptosis, with long-term use, the 2:46 predominant effect 2:48 of glucocorticoids on the skeleton is actually reduction in bone formation. 2:54 The decline in bone formation is mediated by direct inhibition of osteoblasts 2:59 proliferation 3:00 and differentiation, and by an increase in the apoptotic rate of mature osteobl 3:07 asts and 3:07 osteocytes. 3:11 By glucocorticoid levels, stimulate rank-ligon synthesis by pre-osteoblasts, 3:17 supporting osteoclasts 3:19 differentiation and net bone resorption. 3:23 Normally, there's this molecule called osteoprotegeren, which regulates this 3:28 osteoblast-osteoplast 3:30 interaction by binding to the rank-ligon preventing osteoclasts stimulation, 3:37 essentially. 3:38 However, glucocorticoids increases osteoclastic activity by suppressing 3:44 synthesis of osteoprotegeren, 3:46 and also by increasing production of rank, which is required for osteoclast 3:56 ogenesis. 3:57 So rank-ligon binds onto rank on osteoclasts, stimulating osteoclastic activity 4:03 . 4:04 It becomes active osteoclasts, which will break down bone minerals, and this is 4:09 termed 4:10 bone resorption. 4:18 In summary, glucocorticoids causes bone cell remodeling. 4:22 It reduces bone mass and impairs bone microstructure. 4:28 In addition, glucocorticoids increases bone resorption by decreasing secretion 4:33 of androgens 4:34 and estrogens. 4:39 The net bone resorption, by osteoclasts, reduces bone mineral density and bone 4:45 remodeling, increasing 4:47 the risk of fractures. 4:49 Bone resorption increases serum calcium and phosphate levels due to the 4:54 breakdown of bone 4:55 minerals. 4:57 Now when you have a high serum calcium, the body doesn't want to keep it. 5:02 High serum calcium reduces intestinal absorption of calcium from the gut, and 5:08 also increases 5:10 urinary calcium excretion because you want to get rid of all the calcium in 5:16 your body. 5:17 This will cause hypocalcemia. 5:22 Osteoplasmia will stimulate the parathired gland to release parathired hormone. 5:27 Parathired hormone works by binding onto parathired hormone receptors on oste 5:32 oblasts, which will 5:33 stimulate expression of rank ligand, which will further promote osteoclast 5:38 ogenesis and 5:39 so increase bone resorption further. 5:46 Now indirect glucocorticoid effects that also predispose patients to an 5:50 increased risk 5:51 of fractures include reduced muscle mass and weakness leading to increased risk 6:00 of fall. 6:01 Clinical manifestation of glucocorticoid-induced osteoporosis and fractures. 6:07 Vitibyl fractures are the most common glucocorticoid-induced fractures and are 6:12 often asymptomatic. 6:13 These are diagnosed as an incidental finding on chest or abdominal radiograph. 6:18 In patients who have asymptomatic vertebral fracture, there is often no history 6:22 of preceding 6:23 trauma. 6:24 The typical symptomatic patient presents with acute back pain after sudden 6:28 bending, coughing, 6:30 or lifting. 6:31 Fractures due to glucocorticoid use occur at high bone mineral density values 6:35 that occur 6:36 in postmenopausal osteoporosis. 6:40 Remember on a side note, glucocorticoids can cause a vascular necrosis. 6:47 The risk factors for having fractures associated with glucocorticoids include 6:52 advanced age, 6:53 larger steroid doses, longer duration of glucocorticoid therapy, an increased 6:59 risk of fracture has 7:00 been reported with doses of steroids, glucocorticoids, as low as 2.5 to 7.5 7:07 milligrams daily. 7:10 And so knowing the risk of fractures and osteoporosis associated with glucocort 7:15 icoid, it's important 7:17 to prevent the fractures. 7:19 So anyone on steroids should do weight-bearing exercises to prevent both bone 7:24 loss and muscle 7:25 atrophy. 7:27 Patients should avoid smoking and excessive alcohol intake. 7:33 Patients should take measures to prevent falls as well by using a walking stick 7:36 or walking 7:37 frame. 7:39 Vitamin D and calcium supplements can be effective. 7:44 Microchological management can also be used, and indications to use drugs 7:50 include already 7:51 having a fracture, a frailty fracture. 7:55 If someone already has osteoporosis, and if they're above 50, both men and 8:00 women, and 8:01 if someone is taking glucocorticoids and has diagnosed osteoporosis with a T 8:07 score of 8:07 less than negative 2.5. 8:12 Dysphosphonates are first line to prevent osteoporotic fractures. 8:18 The side effects of dysphosphonates include reflux and esophagitis, for example 8:23 . 8:24 And so you have other second-line treatments, such as parathyroid hormone 8:29 analogs, or denusumab, 8:31 which is a monoclonal antibody against rank ligand. 8:36 Interestingly enough, if someone is on denusumab, which is 6-monthly injections 8:41 , there's an 8:41 increased risk of vertebral fractures if you stop taking denusumab, and so it's 8:46 important 8:47 to transition safely to bisphosphonates, for example. 8:52 Bisphosphonates directly affect osteoplastic activity, inhibiting bone reabsor 8:58 ption. 8:58 Parathyroid hormone analogs, weirdly enough, actually has a net effect that 9:04 reduces osteoplastic 9:05 activity. 9:08 Dysphamab is a monoclonal antibody that binds to rank ligand and so it inhibits 9:13 the rank 9:14 ligand and rank interaction. 9:18 In summary, glucocorticoid-associated osteoporosis and fractures typically 9:23 occur more so in the 9:25 elderly at large doses of glucocorticoids and longer duration of glucocorticoid 9:30 use. 9:30 The most common side of fractures associated with glucocorticoid use is the 9:35 vertebral 9:35 column, and also usually asymptomatic. 9:40 First-line treatment for prevention are bisphosphonates.