Obstructive Sleep Apnoea

Sleep apnea syndrome is an extremely common medical disorder associated with important morbidity. Sleep Apnea and can be classified as:
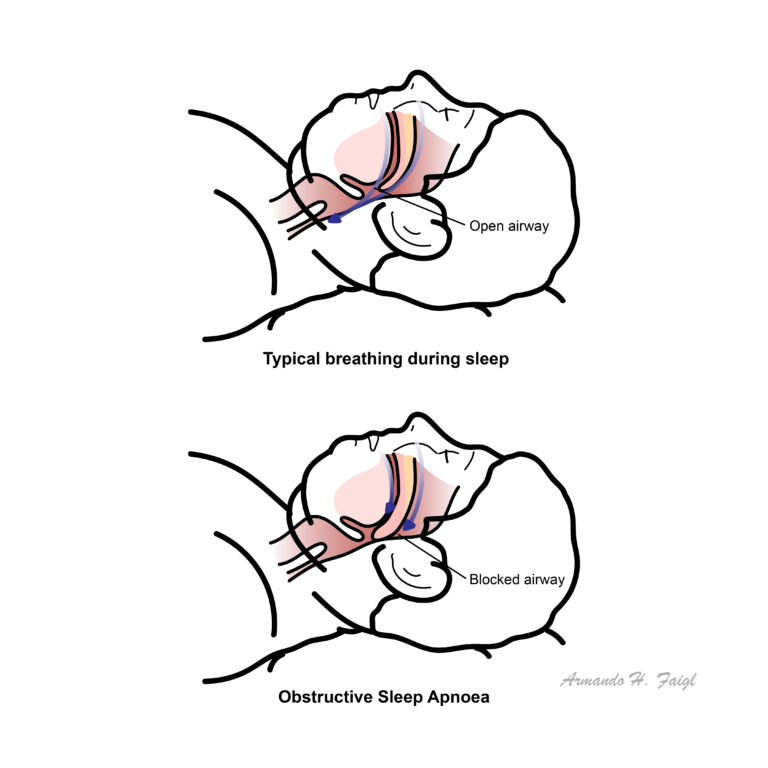
Apnea:an episode of breathing cessation lasting at least 10 seconds in duration.
Hypopnoea: ≥10 second 50% reduction in breathing.
This page will mainly focus on Obstructive Sleep Apnoea.
Other risk factors
Clinical Features Typically an obese middle ages man who presents because of snoring and feeling tired during the day. Partner describes periods of apnoeic attacks.
Examination
Investigation
The diagnosis of Obstructive Sleep Apnoea is based upon the presence or absence of related symptoms & the frequency of respiratory events during sleep (apneoas, hypopnoeas & respiratory effort related arousals) as measured by polysomnography or home sleep apnoea testing.
Severity Currently, the apnea–hypopnea index (AHI, number of apneas and hypopneas per hour of sleep) is the standard metric used to describe the severity of sleep apnea
| Mild | Moderate | Severe |
| 5-15 apnoeic episodes | 15-30 apnoeic episodes | >30 apnoeic episodes |
| Relatively asymptomatic | Aware of daytime sleepiness & take steps to avoid falling asleep at inappropriate times | Daytime sleepiness that interferes with normal activities. |
Obstructive Sleep Apnoea Management
Medical Interventions
Adherence:Estimated that 20-40% of patients do not use their positive airway pressure device & many others do not used it all night, every night.
Surgical therapy
Pharmacology
Patients continuing to have excessive daytime sleepiness despite adequate OSA-specific therapy may benefit from adjunctive pharmacologic therapy to stimulate respiratory drive:
Theophylline, an xanthine derivative chemically similar to caffeine and theobromine, is used to treat asthma and bronchospasm. Theophylline relaxes the smooth muscle of the bronchial airways and pulmonary blood vessels and reduces airway responsiveness to histamine, methacholine, adenosine, and allergen. Theophylline competitively inhibits type III and type IV phosphodiesterase (PDE), the enzyme responsible for breaking down cyclic AMP in smooth muscle cells, possibly resulting in bronchodilation. Theophylline also binds to the adenosine A2B receptor and blocks adenosine mediated bronchoconstriction. In inflammatory states, theophylline activates histone deacetylase to prevent transcription of inflammatory genes that require the acetylation of histones for transcription to begin. Side effects: Nausea/vomiting, stomach/abdominal pain, headache, trouble sleeping, diarrhea, irritability, restlessness, nervousness, shaking, or increased urination.
Central sleep apnoea: (ranked in order of treatment line)
Without Cheyne-Stokes breathing:
With Cheyne-Stokes breathing:
Cheyne-Stokes breathing is a disorder characterised by recurrent central apnoeas during sleep alternating with a crescendo-decrescendo pattern of tidal volume. It is often observed in patients with congestive heart failure and severe sleep apnoea.
Acetazolamide is a reversible inhibitor of the carbonic anhydrase enzyme that results in reduction of hydrogen ion secretion at the renal tubule and an increased renal excretion of sodium, potassium, bicarbonate, and water. It can be used as a diuretic or to treat glaucoma as it prevents excessive build up of aqueous humor. It also inhibits carbonic anhydrase in the central nervous system to minimize abnormal and excessive discharge from CNS neurons. Acetazolamide can be administered to patients with a metabolic alkalosis to promote retention of hydrogen ions at the level of the renal tubule. Side effects: dizziness, lightheadedness, polyuria, blurred vision, dry mouth, drowsiness, loss of appetite, stomach upset, headache, fatigue, tinnitus.
Type II respiratory failure is where you have ↑CO2 and ↓O2. Initial treatment is thus BiPAP).
Patients efficiently treated may report improvements in alertness and some improvement in quality of life, mood, and cognitive function. Mortality and morbidity from cardiovascular disease is also reduced. Risk of motor vehicle accidents seems to be lower in treated versus untreated patients.

Please confirm you want to block this member.
You will no longer be able to:
Please allow a few minutes for this process to complete.
Discussion