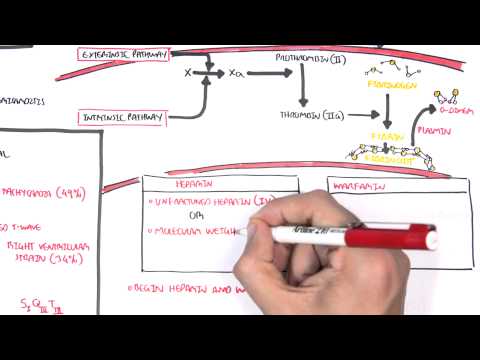
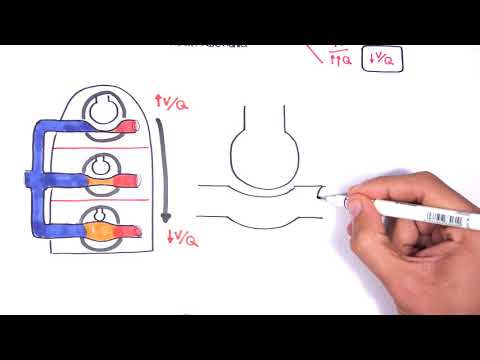
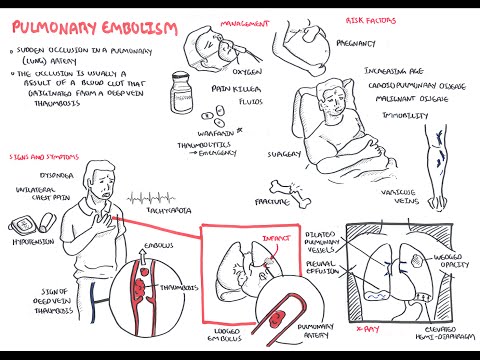
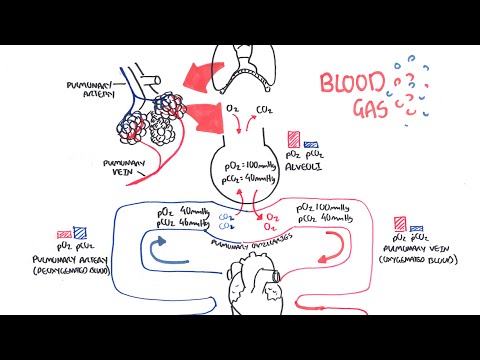
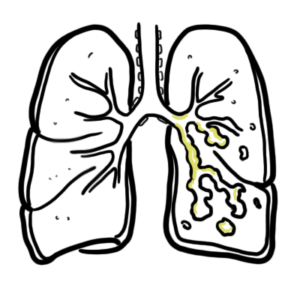
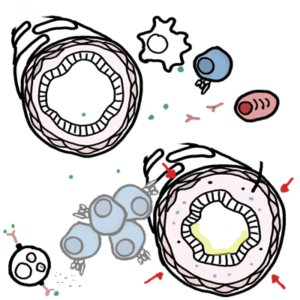
0:00 So, in this video, we're going to talk about pulmonary embolism, and we're 0:09 going to look 0:10 at the signs and symptoms, the risk factors, the pathophysiology, the 0:16 investigations, the 0:17 diagnosis, and then we look at the treatment, the management. 0:20 So, it's a complete video looking at pulmonary embolism. 0:24 So, here, I'm drawing a person who has pulmonary embolism. 0:27 I'm drawing the heart, the lungs, the inferior vena cava, and the descending a 0:34 orta. 0:35 The signs and symptoms of pulmonary embolism include dyspnea, pleuritic chest 0:40 pains, tachycardia, 0:42 hypotension, and signs of deep vein thrombosis, which includes a swollen leg 0:48 and pain in 0:49 the legs, the lower legs. 0:52 And deep vein thrombosis is very important because it's one of the causes of 0:58 pulmonary 0:59 embolism. 1:00 About 95% or 90% of pulmonary emboli is a result of a thrombosis that occurs 1:07 from the deep veins. 1:09 But there are other risk factors that can lead to pulmonary embolism, and these 1:13 are 1:14 surgery such as major abdominal and pelvic surgeries, orthopedic surgeries, 1:20 dead tricks 1:21 such as pregnancy being pregnant, cardiorespiratory problems such as COPD and 1:26 congestive heart 1:28 failure are also risk factors, lower limb problems such as varicose veins, 1:33 fractures, 1:34 malignant diseases, increasing age, immobility, and lastly, thrombotic 1:39 disorders. 1:40 So, these are the risk factors that can lead to pulmonary embolism or pulmonary 1:46 emboli. 1:47 Thrombotic disorders is what we will focus on because, as I mentioned, 95% of 1:52 cases of 1:52 pulmonary embolism is a result of thrombosis from the deep veins. 1:58 So, where do these thrombose, thrombia occur? 2:01 Will they occur from, mainly from the lower limb deep veins, and these include, 2:08 you know, 2:09 women and less common ones. 2:10 So the common ones are your external iliac vein, your femoral vein, your deep 2:16 femoral 2:17 vein, your popliteal vein, your posterior tibial vein, and then the less common 2:21 sites 2:22 where thrombia can occur, and that can lodge into the lungs, are your right 2:27 sided, from 2:28 your right side of the heart, gonatal veins, uterine veins, and your great sa 2:33 phenous. 2:34 So, again, these are sources where thrombia can occur, and then break off 2:41 lodging into 2:42 your pulmonary arteries, causing pulmonary embolism. 2:46 So, what is a thrombose, a thrombia? 2:49 Well, let's zoom into this, let's just say, this external iliac vein, and here 2:54 I'm drawing 2:54 the external iliac vein, and thrombia, a thrombose is essentially a collection 2:58 of red 2:58 blood cells all clumped together with platelets and fibrin. 3:02 So, here I'm drawing this to represent a thrombus, so here we have a vein, and 3:10 this red thing 3:11 is the thrombus, so that's a representation of a thrombus. 3:15 And thrombus is caused by a variety of things, mainly cause, the main cause of 3:22 it is known 3:23 as virtuose triad, and this essentially is a triad of things that leads to a th 3:30 rombus 3:30 formation. 3:31 So, just to recap what a thrombus is, it's essentially, again, you got red 3:36 blood cells 3:36 clumping together with platelets, and then you have fibrinogen, which is a clot 3:41 ting factor, 3:42 which gets converted by thrombin, which is 2A here, into fibrin, and then you 3:50 get these 3:50 fibrin, fibrin, fibrin, meshwork, all like clumping together, causing a throm 3:57 bus formation. 3:58 And again, virtuose triad are a triad of things that essentially promotes throm 4:03 bus formation, 4:04 and these three things are, one, abnormal blood flow, such as absence of blood 4:11 flow, 4:12 two, hyperquagulability, such as thrombophilia, and three, altered vessel wall, 4:18 abnormal vessel 4:19 wall. 4:20 So again, these three things, which make up virtuose triad, promote thrombus 4:27 formation. 4:27 Once a thrombus is formed, it has a few fates. 4:31 We will talk about five in this video. 4:36 Thrombus can just resolve, so it can disappear, so resolution is one outcome. 4:42 The second outcome is propagation. 4:44 The thrombus can just keep growing along the vein. 4:47 Three, the thrombus can break off, lodge, forming an emboli, so embolism. 4:53 A thrombus can also re-canulize, essentially having holes in it, changing its 4:59 structure, 4:59 and then it can organize organization, and this essentially means when the th 5:03 rombus goes 5:04 within the layers of the vessel wall. 5:09 In this video, we will mainly focus on embolism, so when the thrombus breaks 5:14 off. 5:14 So in this diagram here, you can see an embolus, an emboli, which broke off, 5:20 and it will travel 5:21 up to the inferior vena cava and then up towards the heart. 5:26 So here I'm drawing the heart, and here I'm drawing the lungs. 5:31 So the emboli travels up, it goes into the right atrium, then goes down to the 5:36 right ventricle, 5:38 and then it goes up the pulmonary trunk, and it can go either way to the 5:42 pulmonary arteries. 5:44 Let's just say it lodges here, so this is a pulmonary emboli. 5:49 It has lodged into one of the smaller branches of the pulmonary artery. 5:55 We will now look at the pathophysiology. 5:59 So a pulmonary embolism can lead to, depending on how big it is, an increase in 6:05 pulmonary 6:06 vascular pressure. 6:08 An increase in pulmonary vascular pressure causes slight back flow of blood to 6:13 the right 6:14 side of the heart. 6:16 And this will lead to an increase in right ventricular pressure. 6:21 An increase in right ventricular pressure will dilate the ventricles, it will 6:25 cause 6:25 dilation of the right ventricle, which can subsequently lead to right-sided 6:31 heart failure. 6:32 When you have right-sided heart failure, it will obviously decrease the stroke 6:37 volume 6:37 and decrease the cardiac output, and so it logically decreased the blood 6:43 pressure. 6:43 And this is on the right side of the heart, remember, but whatever happens on 6:47 the right 6:47 side of the heart, it will also affect your left side of the heart. 6:51 And so what you get is, from the left side, you get also a decrease in cardiac 6:57 output. 6:57 So when you have actually a decrease in cardiac output, there will be receptors 7:01 that will 7:01 detect this, and that will stimulate the sympathetic response. 7:06 And the sympathetic response will work to increase heart rate, so you get tachy 7:11 cardia, 7:11 and also cause vasoconstriction, so it will try to increase blood pressure. 7:17 But it won't work. 7:20 The result, the net result would be hypotension, because even if you constrict 7:25 your vessels 7:26 to increase blood pressure, because you have the pulmonary emboli in the 7:32 pulmonary artery, 7:33 you will still get a decrease in cardiac output. 7:35 And so this will have a net decrease in blood pressure, if that makes sense. 7:41 So that was the effects a emboli has on the cardiovascular system. 7:46 Let's see what effects it has in the lungs during respiration. 7:52 So here I'm drawing the alveoli, the pulmonary arteries in blue, and the 7:57 pulmonary veins 7:58 in red. 8:00 Ventilation is the air moving in and out of the lungs, and that's denoted as V, 8:06 and then 8:07 the perfusion is the blood flow to and out of the lungs. 8:11 So this is your tube. 8:16 And here is our emboli, let's just say, that because the emboli lodges here, it 8:20 causes 8:21 two main things. 8:22 Firstly, it causes inflammation, second, it causes VQ mismatch. 8:27 So ventilation, perfusion, mismatch. 8:31 So an pulmonary emboli causes abnormal gas exchange. 8:39 So pulmonary embolism leads to an obstruction, which leads to VQ mismatch and 8:46 inflammation. 8:47 Inflammation results in a lot of cytokines being released, which will lead to 8:53 bronchoconstriction. 8:55 VQ constriction, which decreases the oxygen coming in, and because of this, the 9:03 decrease 9:04 in oxygen will stimulate hyperventilation. 9:06 So you're breathing rapidly, which will lead to hypocapnea, a decrease in 9:13 carbon dioxide. 9:15 So the VQ mismatch and inflammation both contribute to hypoxemia and hypocapnea 9:23 , which leads to 9:25 respiratory alkalosis. 9:29 Respiratory alkalosis is what we can find when we do an ABG test, an arterial 9:34 blood gas 9:34 test. 9:35 I hope that made sense. 9:38 So a person presenting with pulmonary embolism, like symptoms, may come in. 9:45 But how do you know it's pulmonary embolism and how do you rule out other 9:50 differentials? 9:51 Well, investigation can be performed, which is what we will look at next. 9:56 So investigations. 9:59 We can do an x-ray. 10:00 Now, x-ray is very important for any respiratory problems. 10:04 But x-rays usually come back normal for pulmonary embolism. 10:08 And x-rays are used to exclude other differentials, such as pneumonia and pneum 10:14 othorax. 10:15 But you can find some common features in pulmonary embolism, in PE. 10:20 So here, let's just draw this x-ray image out, here of the lungs, the mediastin 10:26 um, the heart. 10:28 So one thing you can see is that you can potentially see an enlarged pulmonary 10:32 artery 10:33 because of pulmonary vascular increase in pressure. 10:36 Two, you can see a wedged shaped opacity, which is somewhat like a 10:42 consolidation, but 10:44 it's due to infarction of that area. 10:46 There's no blood supply to that area due to the embolie. 10:50 Three, you can see an elevated hemidiaphragm. 10:52 And four, you can see a pleuridic effusion. 10:57 The second investigation you can do, which should be done, is ECG. 11:01 This also usually comes back normal, but it's used to exclude myocardial infar 11:07 ction and 11:08 pericarditis. 11:09 But you do find some common findings in PE, in pulmonary embolism. 11:14 So let's have a look. 11:16 So here I'm drawing an ECG sort of image strip, but we're only looking at just 11:21 the main ones. 11:22 So in lead two, let's just look at what a normal ECG looks like. 11:27 We have this, it looks like this. 11:29 We have the PQRST wave, and between the RR interval is your rate. 11:36 And the rhythm should be normal, right? 11:39 Well in PE, you can see sinus tachycardia in about 50% of cases. 11:44 And this is essentially when your rate increases, so your RR interval shortens. 11:50 And this you can see in lead two. 11:53 Another thing you can see in PE, in about 35% of cases, is right ventricular 11:58 strain. 11:58 And right ventricular strain can be seen in leads V1 to V4. 12:03 And essentially if we draw it out, what you see is that the T-wave is inverted. 12:09 Of course in the ECG, this doesn't actually look like this, the actual PQRST 12:15 wave. 12:16 But the T-wave is inverted for right ventricular strain. 12:21 Another thing you can see in ECG is what's known as a S1 Q3 T3. 12:25 And you're essentially looking at leads V1 and leads V3. 12:29 And what you're seeing is that you're seeing deep, deep versions of this wave 12:34 in that lead. 12:35 So for example, for lead one, you see a deep S-wave. 12:40 So the S-wave is deeper than usual. 12:43 In leads three, you see a deep Q-wave and you see a deep T-wave. 12:48 I hope that made sense. 12:50 Other investigations that can be performed is your CT pulmonary angiogram, 12:54 which is a 12:54 gold standard for finding out if the person has PE. 12:59 You also have, you can also do a VQ perfusion scanning test, which is used, 13:03 what I mean 13:04 by not really used is that people, it's not definite using that. 13:10 You usually use a CT pulmonary angiogram. 13:12 Five, you can do a bedside echocardiogram. 13:15 And six, you can do a D-dimer assay, which we will look into in more detail 13:22 next soon. 13:24 Okay, so diagnosing or the clinical signs of PE is very difficult to 13:30 differentiate from 13:32 other differentials. 13:35 So what's important when trying to see if a person has PE, it's important to 13:40 look at 13:40 their risk factors.