Overview
Dyspnea (Greek dys, meaning “painful,” “difficult,” and pneuma, meaning “breath. Dyspnea is the medical term for subjective experience of breathlessness or shortness of breath. Dyspnea can be acute when it develops over hours to days and chronic when it has been for more than four to eight weeks.
| CAUSES OF DYSPNOEA | |
| Acute | Chronic |
| Pulmonary edema | COPD |
| Asthma | Left cardiac failure |
| Injury to chest wall and intrathoracic structures | Asthma |
| Spontaneous pneumothorax | Pulmonary vascular disease |
| Pulmonary embolism | Psychogenic dyspnea |
| Pneumonia | Anemia (severe) |
| Acute respiratory distress syndrome | Hypersensitivity disorders |
| Pleural effusion | Pleural effusion |
| Pulmonary Haemorrhage | |
| Foreign body aspiration | |
| Anxiety | |
The usual causes of acute dyspnea in children differ from those in adults. In children, upper airway infection (e.g., epiglottis, laryngitis, or acute laryngotracheobronchitis) is a common cause.
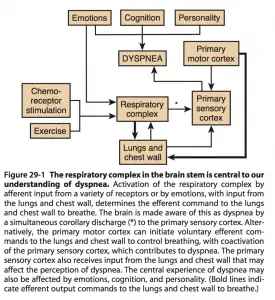
Dyspnea may be due to diseases in virtually any organ system, whether caused by interference with breathing, increased demand for breathing, or weakening of the respiratory pump. In most cases, however, patients with dyspnea can be categorized into one of two groups: respiratory related dyspnea or cardiovascular related dyspnea.
| COMMON CAUSES OF ACUTE DYSPNOEA | |
| Respiratory Disease | Cardiovascular Disease |
| Pulmonary Embolism | Acute left ventricular failure (heart failure) |
| Pulmonary Infection (Pneumonia, bronchitis) | Acute Coronary Syndrome |
| Pneumothorax | |
| Upper airway obstruction (Aspiration, anaphylaxis) | |
| COPD/Asthma exacerbation | |
| LIFE-THREATENING DYSPNOEA | |
| Acute onset Dyspnea | Associated signs/symptoms |
| Foreign object | Sign of choking, Inspiratory and expiratory stridor |
| Anaphylaxis | Angioedema, stridor, rash, pruritus |
| Pulmonary Haemorrhage | |
| Pulmonary Embolism | Acute dyspnea, fever, haemopytsis, pleuritic chest pain, signs of DVT |
| Pneumothorax | Acute dyspnea, one sided-pleuritic chest pain |
| Cardiac Tamponade | Cardinal Quatrad: hypotension,↑JVP, tachycardia, pulsus paradoxus |
| Acute Coronary Syndrome | Retrosternal chest pain, radiates to jaw/neck, diaphoresis and feeling of impending doom |
| Gradual onset Dyspnea | Associated signs/symptoms |
| Asthma exacerbation | Pallor/Cyanosis, ↑resp rate, accessory muscle use, wheezing, silent chest, muscle exhaustion |
| COPD exacerbation | |
| Anaemia | From Haemorrhage: Shock |
| Epiglottitis | “Barking cough” |
| Diabetic ketoacidosis | History of polyuria, polydipsia, polyphagia, and progressive weakness; signs of severe disease include hyperventilation, altered mental status, and abdominal pain |
Approach
- History
- Drugs history
- Amiodarone
- Methotrexate
- Drugs history
| Pharmacology Amiodarone is a K+ channel blocker (class III antiarrythmic). It acts on the myocardium to delay repolarization and increase duration of the action potential. It also decreases SA and AV conduction rate. Side effects (6Ps): Prolongs action potential duration, Photosensitivity, Pulmonary fibrosis and inflammation, Pigmentation of skin, Peripheral neuropathy, Peripheral conversion of T4 to T3 is inhibited (Hypothyroidism). |
- Examination
- Smoker signs
- BMI
| NYHA classification of dyspnea (For Heart Failure) | |
| I | nil at rest, some on vigorous activity |
| II | nil at rest, dyspnea on moderate exertion |
| III | mild dyspnea at rest, worse on mild exertion |
| IV | significant dyspnea at rest and worse on slight exertion |
| MRC Dyspnea score | |
| 1 | Not troubled by breathlessness except on strenuous exercise |
| 2 | Dyspnea when hurrying or walking up a slight hill |
| 3 | Walks slower than contemporaries on level ground due to dyspnea, or has to stop for breath when talking at own pace |
| 4 | Stops for breath after walking 100m or less on ground level |
| 5 | Too breathless to leave house, or when getting dressed |
Investigation
- Pulse oximetry
- Full Blood Count
- EUC
- Electrolytes
- Cardiac troponin
- Brain natriuretic peptide (BNP) or N-terminal pro-BNP
- D-dimer
- Chest X-ray
- Electrocardiogram (ECG)
Specific Dyspnea
- Orthopnea – dyspnea when lying flat. patient usually sleeps with multiple pillows
- Paroxysmal nocturnal dyspnea – episodes of breathlessness at night. It is associated with pulmonary oedema
- Cheyne–Stokes breathing is characterized by alternating periods of hypoventilation and hyperventilation
- Kussmaul breathing – Diabetic ketoacidosis who manifests with “air hunger”: rapid breathing
- Hyperventilation – dysfunctional breathing, breathing off CO2 causes ↓CO2 and so increases pH



Discussion