Percarditis

Pericarditis is the most common form of pericardial disease and a relatively common cause of chest pain. The etiology of pericarditis may be infectious (eg, viral and bacterial) or noninfectious (eg, systemic inflammatory diseases, cancer, and post-cardiac injury syndromes). Tuberculosis is a major cause of pericarditis in developing countries but accounts for less than 5% of cases in developed countries, where idiopathic, presumed viral causes are responsible for 80% to 90% of cases. The diagnosis is based on clinical criteria including chest pain, a pericardial rub, electrocardiographic changes, and pericardial effusion.
Acute pericarditis: An inflammation of the pericardial sac surrounding the heart.
Pericardial friction rub: Harsh, high-pitched, scratchy sound, with variable intensity, usually best heard at the left sternal border by auscultation, due to pericarditis.
Pericardial Effusion: Fluid that fills the pericardial space, which may be due to infection, haemorrhage, or malignancy. A rapidly accumulating effusion may lead to cardiac compromise.
Cardiac Tamponade: Increased pressure within the pericardial space caused by an accumulating effusion, which compresses the heart and impedes diastolic filling.
The pericardium is a membranous layer that covers the heart and helps protect it, fixes the heart in the mediastinum and lubricates the heart.
The pericardium has two layers:
The pericardium has two layers:
Patients with systemic autoimmune disease can have multiorgan involvement, such as pericarditis, nephritis, pleuritis, arthritis, and skin disorders.
Acute Pericarditis triad: chest pain, friction rub and ECG changes.
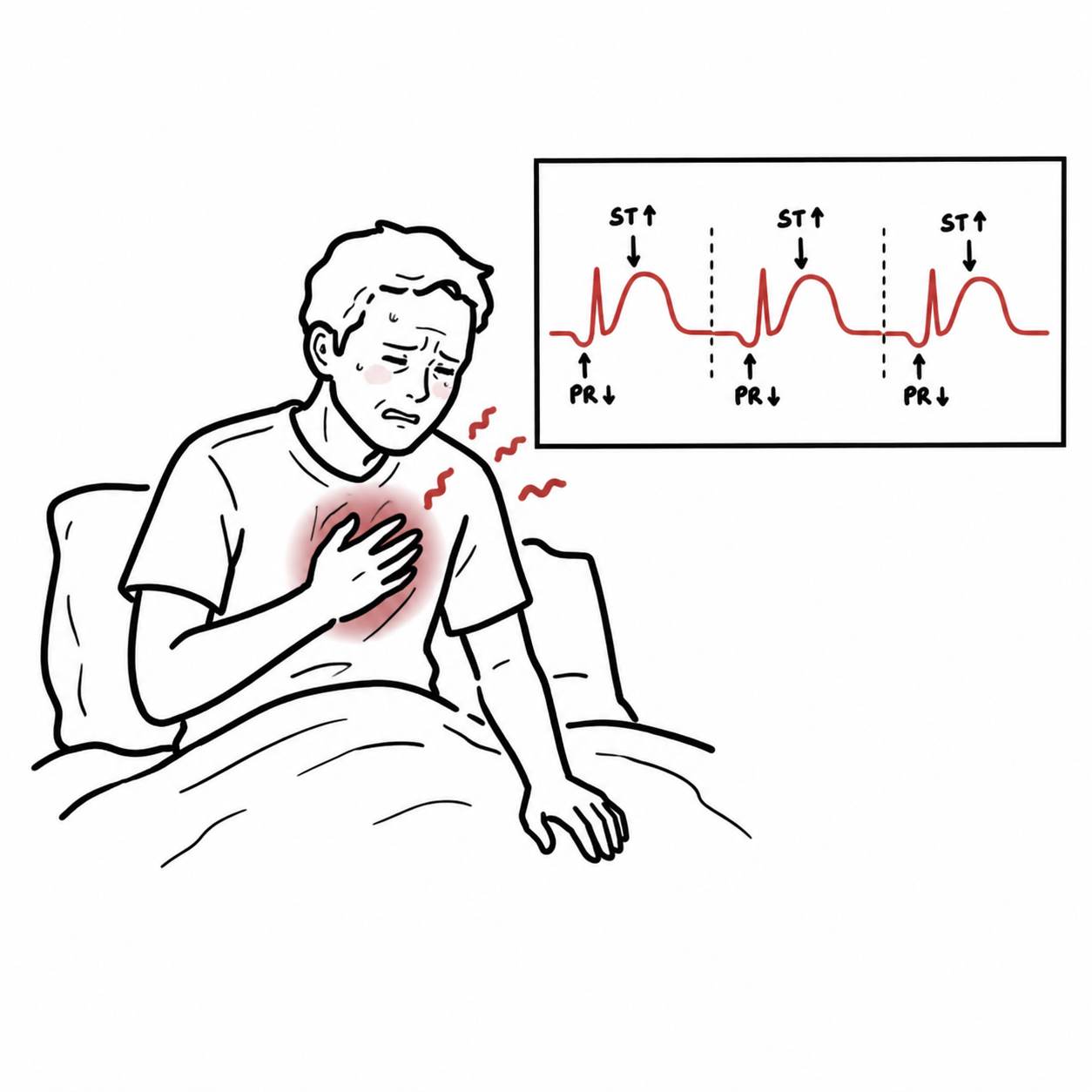
Pericarditis causing pericardial effusion can show
Remember to differentiate pericarditis from other life-threatening causes of chest pain, including acute coronary syndrome, myocarditis or pulmonary thromboembolism.
Prompt echocardiography may be required to determine the presence and amount of pericardial fluid.
| PERICARDITIS VS MYOCARDIAL INFARCTION | ||
| ECG | Acute pericarditis | Acute MI |
| ST-segment elevation | Diffuse in limb leads V2-V6 | Depending on area of infarction (inferior, anterior or lateral) |
| PR-segment depression | Present | Absent |
| QRS complex changes | Absent | Loss of R-wave and development of Q-wave |
In symptomatic pericardial effusion and cardiac tamponade cardiocentesis is performed.
Constrictive pericarditis and pericardial effusion can mimic heart failure but both of these can themselves be differentiated.
| Constrictive Pericarditis | Cardiac Tamponade | Heart failure | |
| Kusmaul’s sign | Present | Absent | Absent |
| Pulsus paradoxus | Uncommon | Present | Absent |
| Jugular Venous Pressure (JVP) | Increased | Increased | Increased |
| Percardial Knock (third heart sound, due to rapid ventricular filling’s being abruptly halted by the restricting pericardium) | Present | Absent | Absent |
| Hypotension | Variable | Severe | Variable |
Kusmaul’s sign looks at JVP relationship with breathing. This is different to Kusmaul breathing which is air hunger, rapid deep breathing a sign of metabolic acidosis.
Constrictive pericarditis may show calcifications of the pericardium on chest x-ray or thickened pericardium on echocardiography. Definitive therapy is resection of the pericardium.
Classical Quatret of Tamponade: hypotension, increased JVP, tachycardia, pulsus paradoxus.
Pathophysiology high intra-pericardial pressure → decreased venous return → decreased diastolic ventricular filling → decreased CO → hypotension and venous congestion Investigation
Managment
Best Practice
UpToDate
Toronto Essential Notes
Oxford handbook of Clinical Medicine

Discussion