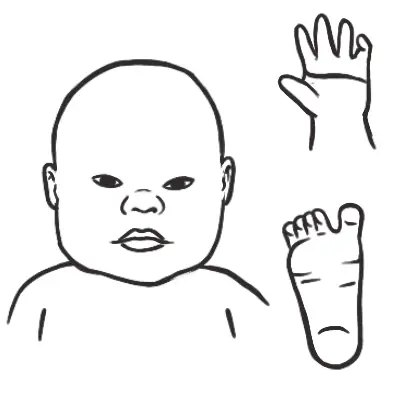
Overview Dysmorphic, which literally means ‘abnormal form’, refers to an unusual appearance, usually of the face. Accurate syndrome diagnosis is important to give information about prognosis, associated problems, recurrence risk and support groups for families. Diagnoses are made by thorough clinical assessment followed by use of aids such as computerized syndrome databases.
| Definition Dysmorphic: Abnormal form, an unusal appearence, usually of the face Syndrome: This is from the Greek ‘running together’ and refers to a cluster of physical and other features occurring in a consistent pattern, with an implied common specific cause that may be unknown. Association: This is a group of physical features that tends to occur together but the link is not consistent enough to allow the term syndrome to be used. An example is the VATER association Sequence: This refers to a group of abnormalities caused by a cascade of events beginning with Definition Types of structural birth defects Malformation arise during the initial formation of the embryo and fetus as a result of genetic and/ or environmental factors during organogenesis (2–8 weeks post-conception). Malformations may include failure of formation, incomplete formation or abnormal configuration. Examples include spina bifida, cleft palate and hypospadias. Disruption result from a destructive process that alters structures after formation. Examples include early amnion rupture causing amputation defects of digits, and vasoconstriction defects caused by cocaine. Deformations result from moulding of a part by mechanical forces, usually acting over a prolonged period. Examples include talipes, congenital hip dislocations and plagiocephaly associated with oligohydramnios. |
History
Antenatal history:
Perinatal history:
Family history
Examination
Pattern of Inheritance
Remember Teratogen is an environmental agent that can cause abnormalities of form or function in an exposed embryo or fetus (examples: sodium valproate and alcohol). Estimated ~ 1% and 3% of birth defects may be related to teratogenic exposure.
|
Common chromosomal disorders
Other common disorders
