Transient Ischaemic Attack (TIA)


Transient ischemic attack is defined as transient neurologic symptoms without evidence of acute infarction. It is a common and important risk factor for future stroke. TIAs are produced by temporary ischemia to a vascular territory, usually caused by thrombosis or embolism and less commonly by vasculitis, hematologic disorders such as sickle cell disease or vasospasm.
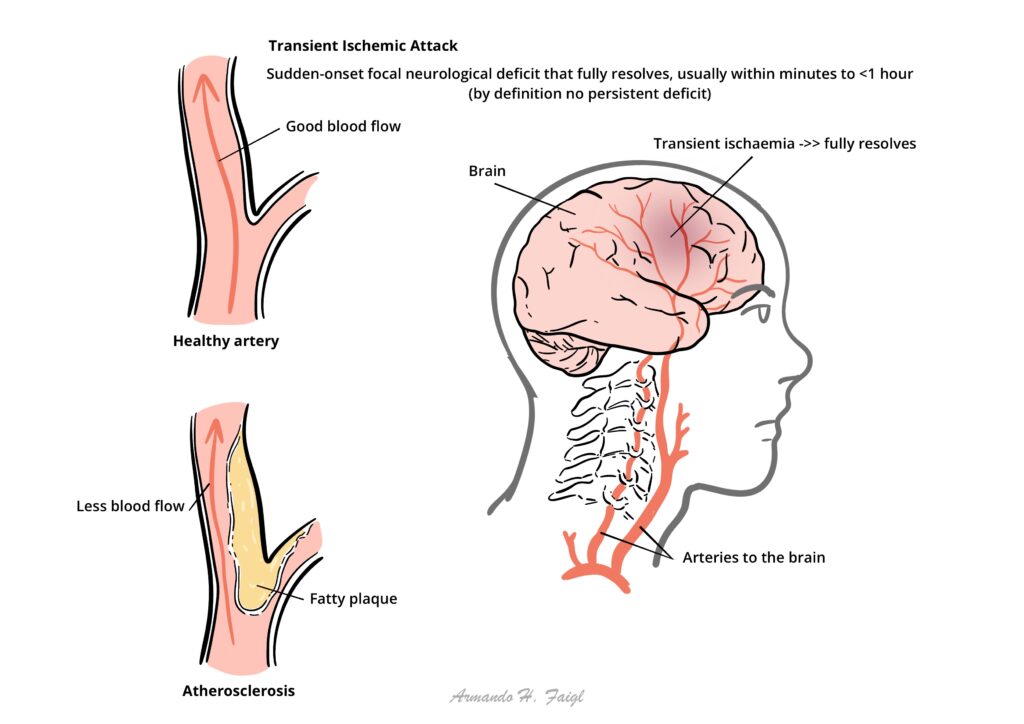
The stroke risk after a TIA is around 10% at 2 weeks, with half of these events occurring within 48 hours. This emphasises the need for rapid clinical assessment and investigations in patients with TIA.
Stroke: Acute onset of a focal neurologic deficit due to a cerebral infarction or hemorrhage.
Transient Ischaemic Attack (TIA): TIA is a transient episode of neurological dysfunction caused by focal brain or retinal ischaemia, without infarction. When there is evidence of brain infarction, the episode is considered to be a mild stroke (if symptoms are minor or disappear).
Amaurosis Fugax: Transient monocular blindness that often is described as a gray shade being pulled down over the eye caused by ischemia to the retinal artery.
Cerebral Anatomy and Blood supply
Sensory Pathways
Motor Pathways
The highest- risk patients for stroke are those with previous ischemic events such as TIA.
The focal neurologic symptoms produced by ischemia depend on the area of the cerebral circulation involved
Many patients with suspected TIA turn out to have a different diagnosis (eg migraine, hypoglycaemia, seizure).
The ABCD (Age, Blood pressure, Clinical presentation, Diabetes mellitus, Duration of symptoms) score should be determined during the initial evaluation and can help assess the immediate risk of repeat ischemia and stroke.
| CONDITION | CLINICAL MANIFESTATION |
| Brain tumor | Severe unilateral headache with nausea and vomiting |
| Central nervous system infection (e.g., meningitis, encephalitis) | Fever, headache, confusion, neck stiffness, nausea, vomiting, photophobia, change in mental status |
| Falls/trauma | Headache, confusion, bruising |
| Hypoglycemia | Confusion, weakness, diaphoresis |
| Migraines | Severe headaches with or without photophobia, younger age |
| Multiple sclerosis | Diplopia, limb weakness, paresthesia, urinary retention, optic neuritis |
| Seizure | Confusion with or without loss of consciousness, urinary incontinence, tongue biting, tonic-clonic movements |
| Subarachnoid hemorrhage | Severe headache with sudden onset and photophobia |
| Vertigo (central or peripheral) | Generalized dizziness and diaphoresis with or without hearing loss |
TIA is more likely with sudden onset, unilateral paresis, speech disturbance, or transient monocular blindness.
TIA and Stroke is a medical emergency!
Imaging
Urgent brain imaging is required. Computerised tomography (CT) can help to exclude a stroke mimic and to differentiate haemorrhagic to ichaemic stroke.
Laboratory investigation
Other (for differentials)
All patients with suspected TIA should get FBC, EUC erythrocyte sedimentation rate (ESR), lipid profile, glucose level, ECG and brain (CT/MRI) and carotid imaging.
| INDICATION FOR CT/MRI |
| Patient on anticoagulants or with abnormal coagulation |
| Plan to give thrombolysis or immediate anticoagulants |
| Deteriorating conscious level or rapidly progressing deficits |
| Suspected cerebellar haematoma, to exclude hydrocephalus |
Medical Management
Aggressive risk factor modification Interventions following a stroke or TIA are aimed at preventing future episodes
In patients found to have a high-grade ipsilateral carotid stenosis, carotid endarterectomy should be performed urgently. The benefit of surgery is greatest within 2 weeks of the TIA or mild stroke as this is the period of greatest risk of recurrent stroke.
Prognosis By definition, a patient with a TIA has no residual symptoms from the primary event.The highest- risk patients for stroke are those with previous ischemic events such as TIA, >10% of TIA patients seen in the emergency department will have a stroke within 3 months.
AAFP – Transient Ischemic Attack: Part I. Diagnosis and Evaluation – 2012
AAFP – Transient Ischemic Attack: Part II. Risk Factor Modification and Treatment – 2012
Best Practice
UpToDate

Please confirm you want to block this member.
You will no longer be able to:
Please allow a few minutes for this process to complete.
Discussion