Diabetes Insipidus

56 year old lady recurrent presentations to your practice for polyuria and increased thirst. Random serum glucose and urinary glucose have returned normal. Patient has otherwise been well, complains of no dysuria, haematuria, fevers or night sweats.
Diabetes Insipidus (DI) is associated with inadequate arginine vasopressin (known as antidiuretic hormone) secretion or renal response to arginine vasopressin, resulting in hypotonic polyuria and a compensatory/underlying polydipsia. There are two main types of diabetes insipidus, central DI and nephrogenic DI
Triad Polyuria, dilute urine, and increased thirst are characteristic of DI.
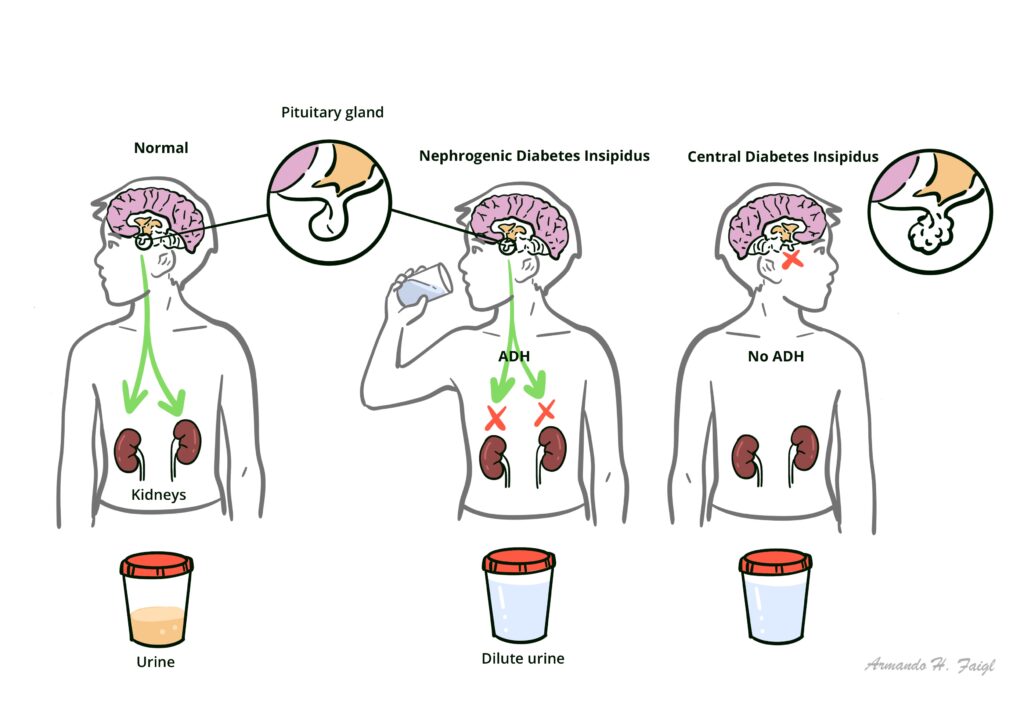
Diabetes Insipidus: Disorder resulting from deficiency of ADH or its action
Diabetes Mellitus: A group of metabolic diseases in which there are high blood sugar levels over a prolonged period.
ADH: Antidiuretic hormone also known as arginine vasopressin
SIADH: inappropriate secretion of ADH (opposite condition to diabetes insipidus)
Desmopressin: artificially acquired ADH (for treatment for those with ADH deficiency/unresponsiveness).
Antidiuretic hormone is initially produced by the hypothalamus and then transported to the posterior pituitary gland via the pituitary stalk for storage.
When osmoreceptors sense hyperosmolarity in the blood it stimulates the posterior pituitary gland to release ADH into systemic circulation.
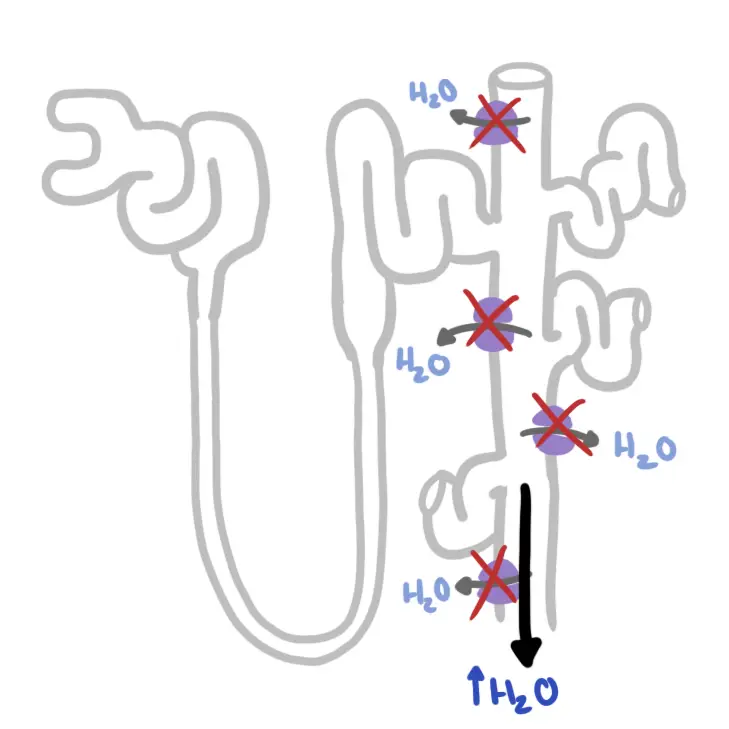
ADH acts on the kidneys and activates the arginine vasopressin 2 (AVP2) receptors of the renal collecting duct which increases the generation of aquaporin 2. Aquaporin 2 channels increases water retention
As a result, there is a net increase in water reabsorption in the collecting duct, leading to appropriate reservation of water and concentrating urine.
To little ADH or lack of response of the kidney to ADH means less water retention and more water output resulting in polyuria.
To little ADH or lack of response of the kidney to ADH means less water retention and more water output resulting in polyuria.
Central DI (also known as neurogenic DI) caused by insufficient synthesis or release of ADH from the central nervous system.
Nephrogenic DI caused by ineffective response to ADH in the kidneys, such as defective ADH receptors caused by genetic defects.
Dipsogenic DI (also known as primary polydipsia) results from excessive fluid intake practiced over an extended period. Sometimes not classified as a true diabetes insipidus.
Gestational DI During pregnancy, vasopressins are more readily metabolised peripherally by placenta hormones. Hence it can provoke transient “central DI” in some patients. Commonly, this condition resolves spontaneously upon delivery.
Wolfram syndrome is a genetic autosomal recessive disorder with the Tetrad: diabetes insipidus, diabetes mellitus, optic atrophy and deafness.
Traumatic or pathological damages affecting the hypothalamus or posterior pituitary gland causes cell death in hormone secreting cells in those areas, thus affecting the normal secretion and release of ADH. Without appropriate stimulation of ADH in the kidneys, renal collecting ducts lost its ability to perform adequate water reabsorption essential for volume maintenance of the body, resulting in a diuretic phenomenon.
Nephrogenic DI is caused by defective ADH receptors in the kidneys. Normally, two receptors AVPR1 and AVPR2 responds to increasing levels of ADH in the systemic circulation. AVPR1 is responsible for vasoconstriction and prostaglandin release, whereas the AVPR2 receptors mediated the antidiuretic response as well as certain coagulation factors (factor VIII and von Willebrand’s factor), hence unresponsive AVPR2 receptors in nephrogenic DI causes diuretic effects as well as mild coagulation defects.
Elevated serum sodium with hypotonic urine strongly suggest DI, serial measures are necessary.
For patients with significant underlying aetiology, DI typically resolves following the resolution of the underlying condition (e.g. correction of hypercalcaemia may result in resolving the presenting DI). With one exception that for lithium therapy induced DI, the condition is usually irreversible.
For patients with irreversible DI, lifelong follow up with monitoring is necessary, with regular assessments of their fluid status, electrolyte and renal functions. They are generally stable with good control by desmopressin, and if indicated, pituitary hormone replacement.

Discussion