Polycystic Kidney Disease
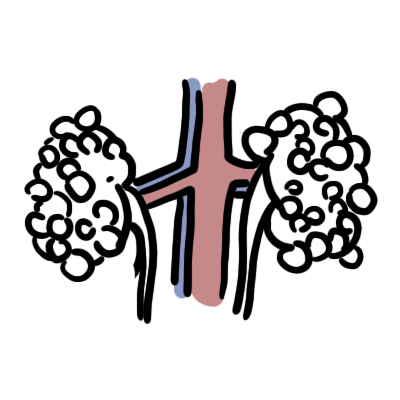

The polycystic kidney diseases are among the most common life-threatening inherited diseases worldwide and frequently cause kidney failure. Autosomal dominant polycystic kidney disease (ADPKD) is seen predominantly in adults, whereas autosomal recessive polycystic kidney disease (ARPKD) is mainly a disease of childhood. For ADPKD, screening asymptomatic at-risk adults with a family history by ultrasound is considered beneficial enabling earlier treatment of complications and to outweigh the risks.
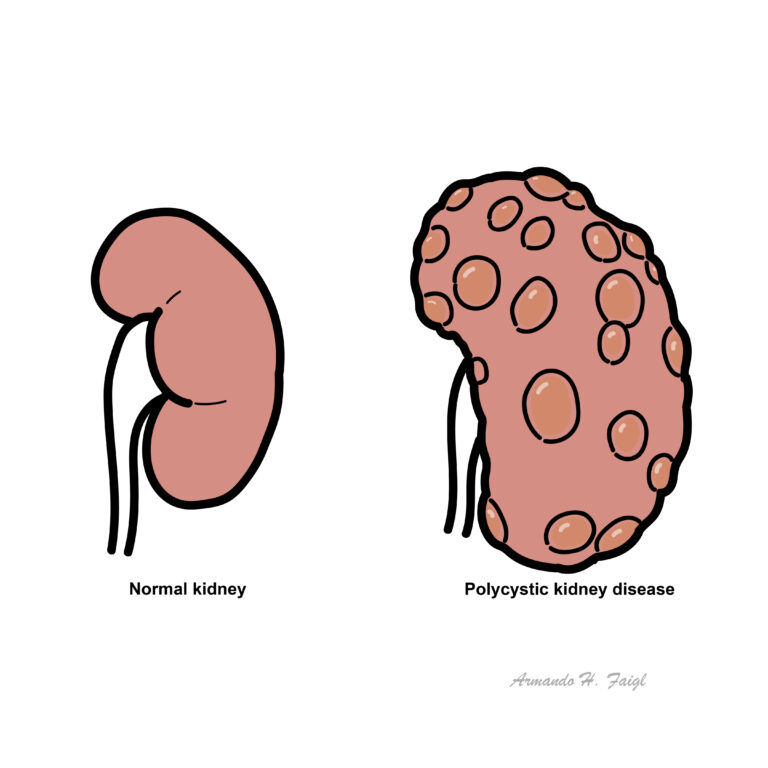
This section will mainly focus on Autosomal Dominant Polycystic Kidney Disease (ADPKD)
Anatomy
The kidneys are retroperitoneal bean shaped organs thats sits between vertebral levels T11-L3. The left kidney sits higher then the right kidney and so the left ureter is longer then the right ureter.
The kidneys is divided into three sections:
Arterial Supply
Venous Drainage
Nephrons
The collecting ducts then drain into the Minor calyx → Major calyx → Renal pelvis → Ureter → Urinary bladder.
Physiology of the Kidney
Function:
ADPKD is a genetic condition. In 80% of cases there is a PKD1 mutation and PKD2 mutation in 20% of cases. This results in a mutation of cells which grow and proliferate forming cysts. These cysts eventually die and fibrose resulting in scarring and fibrosis of the kidney.
ADPKD is a inherited kidney disease. It is Autosomal dominant and so the risk of developing ADPKD is 50%. However, some 10-15% of patients diagnosed with ADPKD will report no family history.
| Risk Factors for Progression of ADPKD |
| Genotype |
| Age of end stage renal failure |
| Male |
| Hypertension |
| Urinary tract manifestation before age 35 years |
Clinical Presentation
Hypertension is the earliest manifestation of ADPKD and is preferentially managed with ACE inhibitors or ARBs.
Examination
| Signs of End-stage Kidney Disease |
| Scar in the iliac fossa nad a mass consistent with renal transplant |
| Arteriovenous fistula (haemodialysis) |
| Peritoneal fistula |
| Scar of the neck consistent with parathyroidectomy (renal bone disease) |
Extra-renal Manifestation
Bilateral Renal Enlargement
Von Hippel-Lindau disease is a hereditary condition associated with hemangioblastomas, which are blood vessel tumors of the brain, spinal cord. The disease has an increased risk of developing clear cell renal cell carcinoma and renal cysts.
Most often, the diagnosis of ADPKD is made from a positive family history and imaging studies showing large kidneys with multiple bilateral cysts and possibly liver cysts
Diagnosis Imaging criteria of ADPKD in at-risk individuals
| Age | Cyst Count | Imaging |
| 15-39 | >3 (total) | Ultrasound |
| 40-59 | 2 (both kidneys) | Ultrasound |
| >60 | 4 (both kidneys) | Ultrasound |
| 16-40 | >10 (both kidneys) | MRI |
No treatment has been proved to prevent cyst growth or the decline in kidney function.
Tolvaptan is a selective vasopressin (ADH) receptor 2 antagonist. It inhibits the reuptake of water from the distal nephron’s and is shown to result in a 50% reduction in the annual rate of kidney growth.
avoiding NSAIDs is advised for people with polycystic kidney disease as this drug is a nephrotoxin.
Complications
Psychological impact of ADPKD – 60% experience anxiety and depression.
Overview
ARPKD is primarily a disease of infants and children. The incidence is 1:20,000 births. The kidneys are enlarged, with small cysts, <5 mm, limited to the collecting tubules.
Diagnosis
Ultrasonography reveals large, echogenic kidneys. The diagnosis can be made in utero after 24 weeks of gestation in severe cases, but cysts generally become visible only after birth.
UpToDate
Best Practice
Oxford Handbook of Clinical Medicine
Roslyn, JS 2016,’Autosomal dominant polycystic kidney disease’, The BMJ, vol 352.
Brenner and Rector’s The Kidney 10th Ed.
Harrison’s Nephrology and Acid-Base Disorders 2nd ed.

Discussion