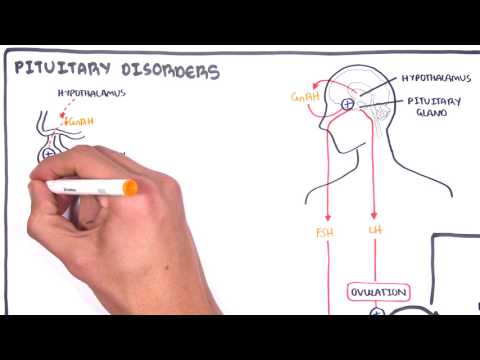
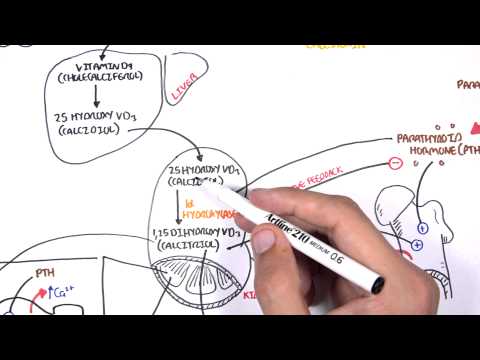
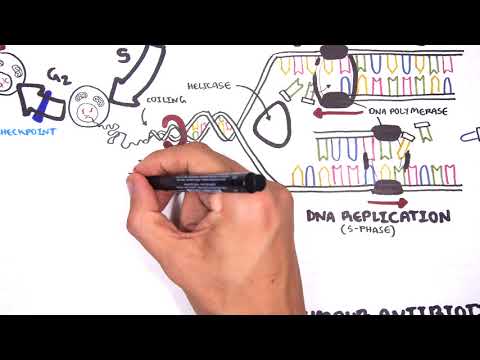
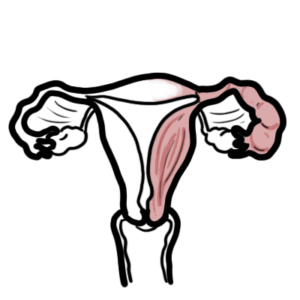
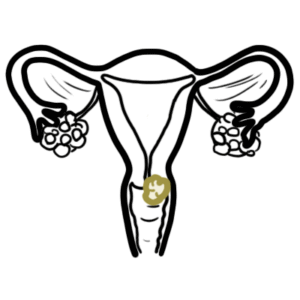
0:00 Armando Hsudunga in Biology and Medicine videos, please make sure to subscribe, 0:05 join 0:05 the forum and group for the latest videos, please visit Facebook, Armando Hsud 0:09 unga. 0:10 In this video, we will look at the hormonal regulation of the female 0:14 reproductive cycle. 0:15 So we will be looking at the menstrual cycle, basically, and yeah, so the 0:21 menstrual cycle. 0:22 The hormones of the female is so much more complicated than the males, but 0:30 hopefully 0:31 we will be able to understand it by the end of this video. 0:34 So we begin with the hypothalamus and the pituitary glands, which are made up 0:38 of the 0:38 anterior and posterior pituitary glands. 0:41 We will be focusing on the anterior pituitary gland. 0:44 The hypothalamus regulates hormones released by the anterior pituitary through 0:49 the portal 0:49 blood here. 0:51 In the female reproductive system, the hypothalamus produces a hormone called 0:56 gonadotropin-releasing 0:57 hormone, which will travel here to the anterior pituitary via the portal blood, 1:03 and it will 1:03 cause the cells in the anterior pituitary gland to produce two important 1:09 hormones, known 1:10 as FSH, follicle stimulating hormone, and LH, luteinizing hormone. 1:18 Please note that in males, this same process also occurs. 1:23 Males also produce gonadotropin-releasing hormone, which will cause the 1:28 anterior pituitary to 1:29 release luteinizing hormone and follicle stimulating hormone. 1:33 So what will these hormones do in the female body? 1:39 Well these hormones will travel to the female ovaries, where the female eggs 1:44 are produced. 1:45 So let's just recap quickly what the ovary is and where it is. 1:51 So here we have the uterus and the ovaries, which connects to the uterus via 1:57 the flopping 1:58 tube, essentially, but it's now known as a uterine tube. 2:03 So we will focus on this ovary here, so let's zoom in. 2:08 So here is the ovary, and it has blood vessels, and it's through these capill 2:14 aries, these 2:15 blood vessels, that the hormones can enter. 2:19 Now in each ovary there are follicles. 2:23 Women have many, many follicles in the ovaries, and each month only some will 2:29 begin to mature, 2:31 that only one will ovulate and become, essentially, will ovulate and produce an 2:39 egg. 2:40 Now let's just say it's the beginning of the menstrual cycle. 2:43 So just after female has shed her uterine wool, just had the period. 2:48 Now within the ovaries, females have many, many, many primordial follicles, and 2:55 each 2:55 month only some of these primordial follicles will mature into primary foll 3:02 icles, and they 3:04 will keep maturing, but only one will ovulate. 3:09 So here I'm drawing one primary follicle, and it's the beginning of the 3:14 menstrual cycle. 3:18 Before we continue on, let's look at the changes of the hormone concentrations 3:25 that 3:25 come from the brain by looking at a graph. 3:28 So here we have a y-axis, which shows the concentration of the hormones in 3:34 blood. 3:34 And on the x-axis is a duration of the female menstrual cycle, which normally 3:40 goes for about 3:41 28 days. 3:43 So the dotted line in the middle is 14 days, which is halfway. 3:49 Now just to simplify things even more, the menstrual cycle can be divided into 3:54 two phases. 3:56 The first 14 days is known as the follicular phase, and the last 14 days is 4:03 known as the 4:04 luteal phase, and this is important to keep in mind. 4:07 So the first is the follicular phase, the second is luteal phase. 4:13 Now initially, in the beginning of the menstrual cycle, there is an increase in 4:16 gonadotropin-releasing 4:18 hormone, secreted by the hypothalamus, because it's the start of the menstrual 4:24 cycle, and 4:24 this should cause a steady increase in follicle-stimulating hormone and lutein 4:31 izing hormone. 4:32 But instead we see an increase and then a slow dropping level of follicle-stim 4:39 ulating hormone, 4:41 and we have a steady level of luteinizing hormone. 4:44 Why is this? 4:46 Well the reason is actually quite complicated, but just hold on to that thought 4:51 and hopefully 4:51 it will make sense. 4:54 So let's go back to the ovary. 4:56 So follicle-stimulating hormone will initially rise, because the follicular 5:03 phase is the 5:04 first phase of the menstrual cycle, follicle-stimulating hormone will enter the 5:09 ovaries, 5:10 and what they will essentially do is stimulate. 5:12 It will stimulate follicle maturation of these primary follicles. 5:19 And so some of these primary follicles will mature into a secondary follicle. 5:25 I'm only drawing one secondary follicle for simplicity. 5:30 While these follicles are maturing, they produce another hormone called 5:34 estrogen. 5:35 Now, estrogen has many effects. 5:39 In the first 10 days of the menstrual cycle, so in the beginning, estrogen has 5:44 a negative 5:45 feedback on the pituitary gland, inhibiting the release of luteinizing hormone. 5:51 To put it simply, at low concentrations, estrogen inhibits luteinizing hormone 5:57 secretion from 5:58 the anterior pituitary. 6:03 And that is why we only see a steady level of luteinizing hormone in the blood, 6:08 because 6:09 even though gonadotropin-releasing hormone from the hypothalamus is stimulating 6:13 the release 6:14 of luteinizing hormone, at low concentrations, estrogen will inhibit lutein 6:20 izing hormone release. 6:24 Another fact is that follicle-stimulating hormone is secreted primarily in 6:29 response to 6:30 low estrogen concentrations. 6:33 So when estrogen levels rise, follicle-stimulating hormone levels will fall. 6:38 And that is why we see in the graph, a steady drop in follicle-stimulating 6:42 hormone, because 6:43 there's an increase in estrogen levels from the follicles. 6:47 So let's draw another graph and see the concentrations of the hormones produced 6:52 by the ovaries during 6:53 the menstrual cycle, which goes on for 28 days. 6:58 So as the follicle matures, they will produce more estrogen, which as I 7:02 mentioned, at low 7:03 concentrations, estrogen will inhibit the secretion of luteinizing hormone, and 7:10 also the increase 7:11 in estrogen concentrations will cause a decrease in follicle-stimulating 7:18 hormone secretion. 7:20 Estrogen is an important hormone, especially for females, because estrogen is 7:25 basically 7:26 male's equivalent of testosterone. 7:30 Estrogen peripheral effects include stimulating bone and muscle growth. 7:35 It stimulates endometrial growth, maintains female secondary characteristics, 7:42 and maintains 7:44 the glands, the breasts, amongst many other things. 7:50 So just to draw this graph up to 10 days of the menstrual cycle, we see a 7:58 steady low concentration 8:00 of luteinizing hormone due to the inhibitory effects of estrogen, remember, in 8:05 the first 8:05 10 days. 8:07 And we also see a steady drop of follicle-stimulating hormone due to the 8:11 increase in estrogen levels 8:12 as well, which has a negative feedback. 8:16 So what happens after 10 days? 8:18 Well after 10 days, estrogen levels will continue to rise as the follicles 8:24 mature in the ovaries. 8:26 And after 10 days, as estrogen levels rise, it will have a positive feedback. 8:32 And it will stimulate the release of luteinizing hormone. 8:38 So at low concentrations, estrogen will inhibit luteinizing hormone secretion. 8:44 However, at high concentrations, estrogen will stimulate luteinizing hormone 8:51 secretion. 8:52 Now things are changing, the increase in gonadotropin releasing hormone and 8:58 estrogen will stimulate 9:01 then luteinizing hormone secretion. 9:06 And you see this massive spike in luteinizing hormone concentration. 9:13 It's this massive luteinizing hormone concentration that will trigger ovulation 9:20 of the most mature 9:22 follicle in the ovary. 9:25 The ovulation of the follicle will release what we know as the female egg, the 9:32 oocyte 9:32 or oocyte. 9:35 After ovulation, the luteinizing hormone levels will drop back down. 9:41 gonadotropin releasing hormone will slowly drop as well. 9:45 Follicle stimulating hormone also had a small spike as a side effect of the 9:49 surge of luteinizing 9:51 hormone release. 9:54 So luteinizing hormone triggers ovulation, an oocyte is released. 9:59 After the follicle ovulates, the follicle will turn into a corpus luteum, which 10:04 is a 10:04 dead follicle basically. 10:06 Now, that is why the first 14 days of the menstrual cycle is called the foll 10:12 icular phase 10:13 because it all has to do with the follicles and its maturation. 10:17 And the last 14 days is known as the luteal phase because we have the formation 10:22 of the 10:22 corpus luteum. 10:27 The corpus luteum will essentially slowly degrade however it also has a purpose 10:34 in that it secretes 10:35 hormones. 10:36 It secretes three hormones, estrogen again, inhibin and progesterone. 10:44 So what we see in the concentration levels of these ovarian hormones, estrogen 10:51 will increase 10:52 until ovulation and then drop slightly. 10:57 Inhibin was not present until after ovulation, then it begins to increase 11:02 thanks to the corpus 11:03 luteum, progesterone levels were low until after ovulation during the luteal 11:12 phase. 11:14 So at 21 days of the female reproductive cycle, progesterone is increasing, 11:20 inhibin is increased 11:23 and estrogen is still detectable. 11:26 And all these hormones are all produced thanks to the corpus luteum. 11:31 So what do these hormones do? 11:34 Well, inhibin has a negative feedback and it will essentially inhibit the 11:38 secretion of 11:39 follicle stimulating hormone. 11:41 Because we are at the luteal phase, we don't need any more follicles to mature 11:46 just yet. 11:47 So that is why inhibin is preventing follicle stimulating hormone release to 11:51 prevent follicle 11:52 maturation. 11:56 So here I wrote as the secondary corpus luteum develops, inhibin secretion will 12:01 suppress 12:02 follicle stimulating hormone release. 12:07 One is the most important hormone in the luteal phase and has many functions, 12:14 one of which 12:15 is having a negative effect on the hypothalamus, inhibiting the secretion of 12:19 gonadotropin 12:20 releasing hormone. 12:22 Now after ovulation during the luteal phase, the progesterone levels will 12:27 increase slowly 12:29 and the estrogen levels will decrease slowly, kind of, and this will suppress 12:34 gonadotropin 12:35 releasing hormone release. 12:41 And so progesterone will inhibit gonadotropin releasing hormone release, which 12:46 will also 12:47 affect the release of luteinizing hormone and follicular stimulating hormone. 12:53 So during the luteal phase, as progesterone and inhibin increase, this will 12:59 essentially 13:00 cause a decrease in gonadotropin releasing hormone, luteinizing hormone, and 13:06 follicular 13:07 stimulating hormone. 13:13 But the main effect of progesterone is that it will stimulate endometrial 13:19 growth. 13:20 The endometrial lining is the lining of the uterus, which will shed each month 13:27 or, or 13:28 the endometrium is where the egg will implant if it's fertilized by sperm. 13:36 Okay, let's just say there was no fertilization because this is just a normal 13:42 menstrual cycle. 13:43 And of course, all good things have to come to an end. 13:47 The corpus luteum in the ovary will degenerate allowing a new set of follicles 13:55 to mature. 13:56 So as the corpus luteum degenerates, all these hormones that were produced by 14:01 the corpus 14:02 luteum, the estrogen, inhibit, and progesterone, they will decrease like so. 14:11 So when the corpus luteum degenerates, progesterone will decrease. 14:18 And this will mean that progesterone cannot inhibit gonadotropin releasing 14:23 hormone release. 14:24 And so gonadotropin releasing hormone levels will increase. 14:28 And this will allow a new menstrual cycle to occur. 14:36 Also because of the decrease in progesterone and estrogen in part means that 14:42 these hormones 14:43 cannot maintain the endometrium, the endometrial lining in the uterus. 14:49 And so the endometrium will shed, and this is known as the period. 14:55 And after the endometrial lining sheds, this allows a new cycle to occur. 15:00 And then you see an increase in gonadotropin releasing hormone again, and the 15:04 cycle continues. 15:05 Hope you enjoyed this video. 15:06 Thank you.