Portal Hypertension Overview
Normal portal vein pressure is 5–10mmHg. Portal hypertension develops when the portal pressure is greater than 12mmHg.
Mechanism of disease
Increased Intrahepatic resistance of blood flow through the liver due to cirrhosis Increased splanchnic blood flow secondary to vasodilation leading to increased portal flow through liver Cirrhosis is the most common cause of portal hypertension.
Portal Vein Anatomy
The portal vein drains blood from the GIT so that nutrition absorbed can first enter the liver Portal vein is formed from the superior mesenteric vein and splenic vein Portal vein ← Superior mesenteric vein + Splenic veinSplenic vein ← inferior mesenteric vein CAUSES OF PORTAL HYPERTENSION Prehepatic Hepatic Posthepatic Portal Vein thrombosis Cirrhosis Budd-Chiari Syndrome Splenic Vein thrombosis Acute hepatitis Constrictive pericarditis Massive splenomegaly Parasitic – Schistomosis Tricuspid Regurgitation
Complications of Portal Hypertension
Gastroesophageal varices Portal Hypertensive gastropathy Splenomegaly Ascites Management
Treat complications above Tranjugular Intrahepatic portosystemic shunt (TIPS) Liver transplantation (definitive) Oesophageal-gastric varices Overview
>75% of patients with cirrhosis will eventually develop varices. Risk of variceal haemorrhage is 5-15% per year, and is related to variceal size. Risk amplified in progressive CPS and presence of red wale marks. Without secondary prophylaxis , re-bleeding occurs in 60-70%, usually within the first 2 years of index bleed. Screening is important.
Mechanism of disease
Varceal haemorrhage results from rupture of the variceal wall due to excessive wall tension. Tension opposes the variceal transmural pressure, which depends upon portal pressure and vessel size . Once variceal wall rupture occurs, the amount of bleeding is mainly related portal pressure.
Major complication of cirrhosis and portal hypertension is gastroesophageal varices with haemorrhage.
Investigations
Gastroscopy CT abdoMRI abdoManagement of varices
Prevention – Screening those at risk with gastroscopyyearly – small varices 2nd yearly – no varices If high risk bleeding (Medium and large varices, Any size with red wale markings):Betablockers – Propranolol (to reduce portal venous pressure) OR Endoscopic variceal band ligation Pharmacology Non-selective BetaBlocker (propranolol) – mechanism of action – Reduction in cardiac output and splanchnic blood flow. It allows unopposed alpha-1 adrenergic receptor activity which results in splanchnic vasoconstriction and reduction in portal pressure.
Acute management of variceal bleed – emergency
Resuscitation Bloods – cross match (aim Hb >70) Monitor Fluid resuscitation Contact gastroenterological/surgical team for emergency gastroscopy IV Proton pump inhibitors IV Somatostatin OR octreotide Consider giving vitamin K and fresh frozen plasma to correct clotting problems Antibiotics – oral norfloxacin OR IV ciprofloxacin Balloon tamponade – for those who can not get endoscopy immediately Endoscopy – first line Repeated sclerotherapy injection Endoscopic variceal band ligation Tranjugular Intrahepatic portosystemic shunt (TIPS) Pharmacology Octreotide is synthesised somatostatin used to treat acromegaly, portal hypertension and reduces side effects of chemotherapy. It is used in acute oesophageal bleed because it is through to cause vasoconstriction of splanchnic circulation.
Ascites Overview
Ascites is accumulation of fluid within the peritoneal cavity. Usually 1-2L of fluid in abdomen before patient is aware of abdominal distention.
Clinical features
Abdominal distention Shortness of breath Hepatic hydrothorax Malnourished Muscle wasting Fatigue and weakness Investigation
Ultrasound CT abdomen Paracentesis Bloods – LFT , FBC, EUC Serum to albumin gradient (SAAG)
>11 – portal hypertension <11 – malignant or infectious Management
Complication
Spontaneous bacterial peritonitis Spironolactone associated hyperkalaemia Paracentesis with high neutrophil count >250 is highly suspicious of spontaneous bacterial peritonitis.
Spontaneous Bacterial Peritonitis (SBP)
Common complication of ascites Usually asymptomatic 25% mortality E-coli main causative agent Paracentesis with high neutrophil count highly suggestive of SBP Treatment :Primary prophylaxis in those with low protein (<10g/L) ascites or bilirubin >50 with impaired renal function Splenomegaly Clinical features
Enlarged spleen Thrombocytopaenia and leukopaenia Complications
Click here for more information on splenomegaly
Hepatorenal syndrome Overview
Renal failure without renal pathology due to renal vasoconstriction Renal vasoconstriction leads to RAAS activation which further causes systemic vasoconstriction Vasodilatation in splanchnic system Diagnosis
Large Ascites High creatinine Types of Hepatorenal syndrome
Type I – decrease eGFR and increase in creatinine within 1-2 weeks of presentation Type II – decrease eGFR with increase in creatinine level but stable Management
Midodrine α-agonist Octreotide IV albumin Liver transplantation Pharmacology Midrodrine is a α 1 -receptor agonist and exerts its actions via activation of the alpha-adrenergic receptors of the arteriolar and venous vasculature, producing an increase in vascular tone and elevation of blood pressure .
Hepatic encephalopathy Overview
Alteration in mental status and cognitive function due to liver failure Clinical diagnosis Precipitating events
Hypokalaemia Infection Increased dietary protein load Electrolyte disturbances Clinical features
Personality change within weeks to months Violent OR Sleepy Ascites Asterixis Mechanism of condition
Gut-derived neurotoxins bypass liver Neurotoxins reach the brain Investigations
Ammonia (does not correlate with severity) Management
Identify precipitating factor and correct it Lactulose OR antibiotics (for those where lactulose is no good) – to promote 2-3 soft stools a day and minimise ammonia production by gut bacteria Zinc supplementation Other complications Bone disease due to Vitamin D deficiency
The liver plays a role in the conversion of cholecalciferol to calcidiolCalicidiol then goes to kidneys to become calcitriol the active form of vitamin D Liver failure means the conversion from cholecalciferol to calcidiol does not occur so there is vitmain D deficiency Vitamin D deficiency leads to hypercalcaemia Liver Transplantation Indications for chronic liver disease
Life threatening complications 2 year mortality of 50% without transplant Diuretic resistant ascites Recurrent hepatin encephalopathy Recurrent CBP Recurrent or persistent gastrointestinal haemorrhage Intractable cholnagitis Hepatorenal syndrome MELD SCORE Stratifies severity of end-stage liver disease, for transplant planning.Factors: Dialysis, bilirubin, INR , SodiumMELD SCORE Mortality rate (3-month) <9 3% 10-19 15% 20-29 30% 30-39 60% >40 >70%
Stratifies severity of end-stage liver disease, for transplant planning.
Acute liver disease (King’s College Hospital Criteria)
Paracetamol induced liver failurearterial pH <7.3 OR all three of the following: INR >6.5, Serum creatinine >300 and Grade III/IV encepalopathy Non-paracetamol induced acute liver failureINR >6.5 OR Three of the following five: age <11 or >40, serum bilirubin >300, jaundice to coma time of >7 days, INR >3.5 and drug toxicity Liver Transplantation of hepatocellular carcinoma (Milan Mazzaferro criteria)
A single nodule <5cm OR 3 nodules the largest of which is <3cm no evidence of gross vascular invasion No metastasis 4 year survival of 75%
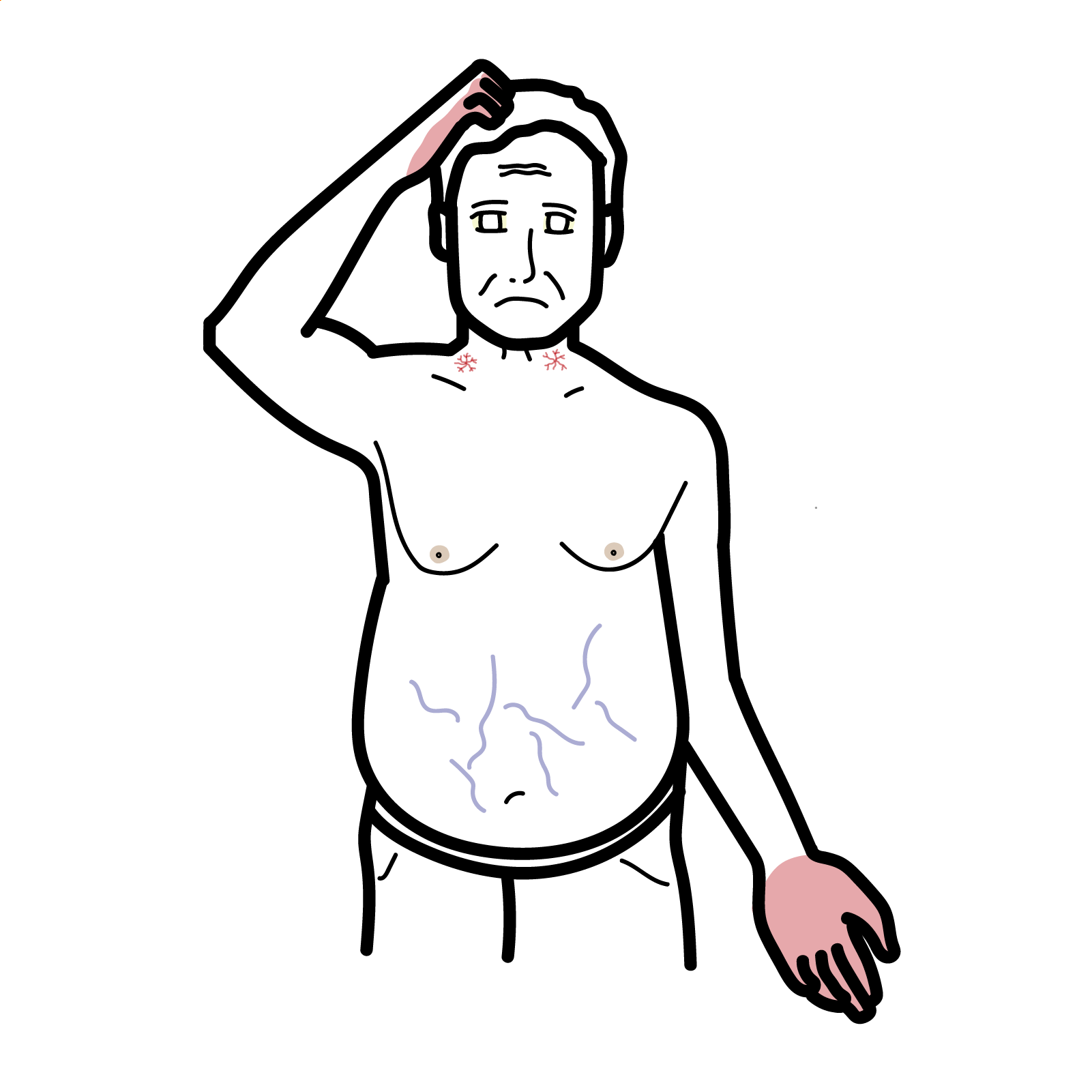

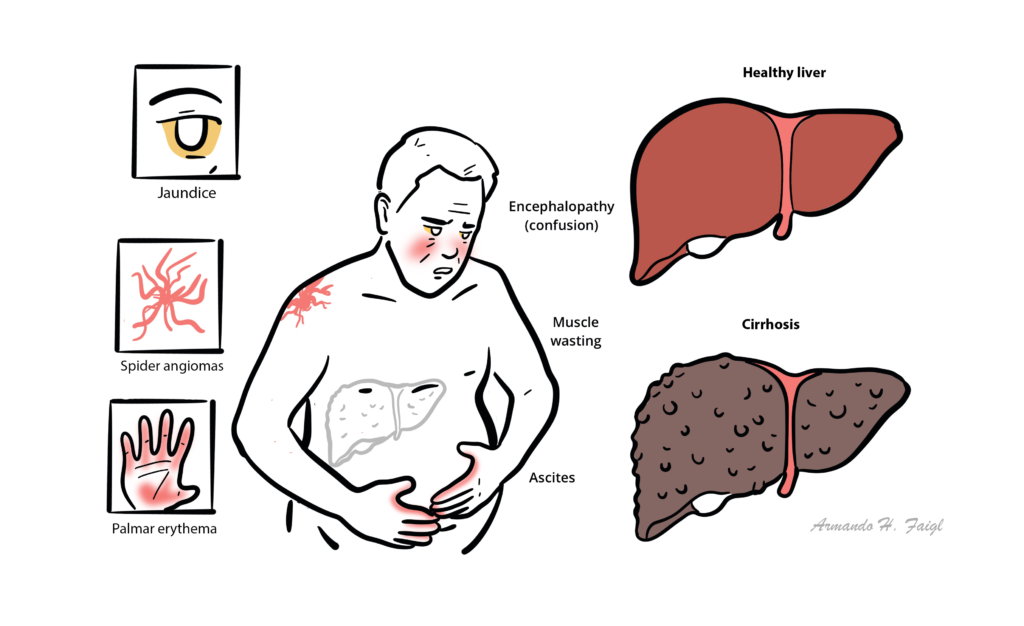

Discussion