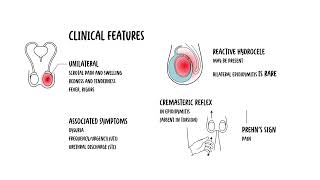
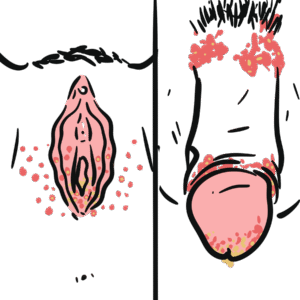
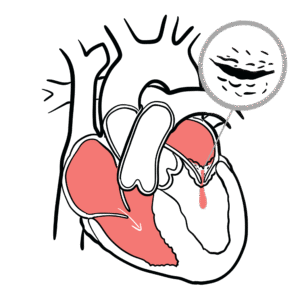
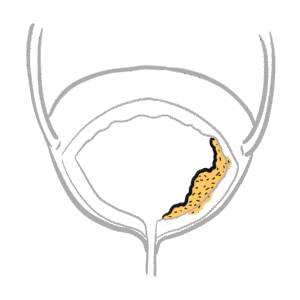
0:00 Epidinomyitis is inflammation of what's called the Epidemus. 0:16 The structure here next to the testicle. 0:20 Inflammation of the testes is called Architis. 0:23 Although people often use the term Epidinomy or Chitis, most cases are 0:28 primarily Epidinomyitis 0:29 and isolated or Chitis is uncommon and usually viral. 0:35 Epidinomyitis has a bi-modal age distribution, it's most common in males aged 0:40 15 to 30 and 0:41 then again in those over 60 reported incidents in the UK is around 25 per 10, 0:50 000 people. 0:52 Let's review some anatomy. 0:55 Think of the testes as the factory that makes sperm, sitting inside a thin bag 1:01 that Chunica 1:02 vaginalis and wrapped in a tough capsule, Chunica alboginia. 1:09 The Epidinomyitis is the storage and maturation tube that hugs the testes along 1:15 the back outside 1:17 posturalateral edge. 1:19 The head sits at the top of the testes, the body of the Epidinomyitis runs down 1:23 the back 1:24 of the testes and the tail sits at the bottom. 1:28 The tail turns into the vast deferens. 1:31 That's the thicker delivery tube that carries sperm away. 1:37 The vast deferens plus the vessels and nerves travels in a bundle called a sper 1:42 matic cord 1:42 which runs up towards the groin. 1:48 Inside the cord you've got many structures. 1:52 The vast deferens as I mentioned, testicular archery, Pepiniform plexus, cre 1:59 mostaric vessels, 2:01 nerves and lymphatics. 2:06 The scrotum which really holds the testes is built in layers like clothing over 2:13 the testes. 2:15 On the outside, skin, darthos, external spermatic fascia, cremostaric muscle 2:25 fascia, internal 2:27 spermatic fascia, Chunica vaginalis and Chunica alboginia. 2:35 The lymph drainage is developmental. 2:38 This is drained up high in paraeotic lumbar nodes, the scrotal skin drains to 2:45 superficial 2:46 inguinal nodes. 2:49 Let's go back to Epidinomyitis which is inflammation of the Epidinamus, this 2:57 area we already spoke 2:59 about. 3:00 Most cases of Epidinomyitis occurs from infection ascending from the lower 3:04 urinary tract, the 3:05 re-thrown bladder, into the Epidinamus. 3:09 The likely organism depends on age and risk factors. 3:13 So, in men under 35, a sexually transmitted cause is most likely commonly chlam 3:20 ydia, trachomyitis 3:21 and niceria gonorrhea. 3:24 In men who practice anal intercourse, enteric organisms like E. coli are also 3:30 common cause 3:31 even if they are under 35. 3:35 So in men over 35, the cause is most often enteric bacteria from a UTI. 3:44 These are E. coli for example, protease, Klebsiella and pseudomonas. 3:51 This is often linked to bladder outflow obstruction like prostate enlargement, 3:56 allowing bacteria 3:57 to ascend and then travel into the Epidinamus causing Epidinomyitis. 4:07 One of the most typical causes of viral archeitis is mumps. 4:12 Archeitis can be a complication of mumps, particularly in post-pubertile males. 4:18 It may occur a few days after paratitis, inflammation of the parotid glands. 4:26 Even with fevers and can be unilateral or bilateral. 4:31 It usually resolves with supportive care but can lead to testicular atrophy and 4:37 infertility. 4:38 If suspected, mumps serology may be required and public health notification may 4:42 apply depending 4:43 on local regulation. 4:49 The risk factors of Epidinomyitis really depends on the likely source. 4:53 Is it sexual transmitted infection in those under 35 or is it a urinary tract 4:58 infection 4:58 or prostate issue in those over 35? 5:02 So risk factors for STI-associated Epidinomyitis, these are multiple partners, 5:07 known contact 5:08 with someone with gonorrhea chlamydia, men who have sex with men unprotected 5:13 sex. 5:14 Urinary tract infection or enteric-associated Epidinomyitis are usually 5:18 associated with recent 5:19 catheterization or instrumentation, bladder outlet obstruction so benign prost 5:24 hetic hyperplasia 5:25 or stricture, recurrent UTIs or someone with an immunocompromised state. 5:34 The typical presentation of someone with Epidinomyitis is unilateral, scrotal 5:39 pain and swelling, 5:40 often with redness and tenderness. 5:42 Fever and rigos may occur. 5:45 Seated symptoms can point to the cause, so disureia, frequency urgency is UTI 5:51 or urethral 5:52 discharges STI, so sexual history is very important. 5:57 On examination, the Epididymus and sometimes the testis are very tender and a 6:03 reactive 6:03 hydroseal may be present. 6:06 Bilateral Epidinomyitis is rare. 6:10 There are some important examinations to perform. 6:13 The cremostaric reflex is usually present in Epidinomyitis but is absent, often 6:20 in something 6:21 called testicular torsion, which is a differential diagnosis. 6:25 There is something called a frinsign where pain relief occurs with elevation of 6:31 the testis 6:32 and can suggest Epidinomyitis, but it's unreliable and not routinely used as a 6:37 decision maker. 6:44 So, while Epidinomyitis is a cause of testicular pain, there are very important 6:50 differentials 6:52 to keep in mind. 6:54 For example, testicular torsion. 6:57 Because testicular torsion is a surgical emergency, torsion typically has 7:01 sudden, severe pain, 7:02 often without urinary symptoms. 7:04 If torsion is a significant certain urgent urologic review and often scrotal 7:08 exploration 7:09 is required. 7:10 Other differentials include trauma, abscess of the testis, Epidinomylcyst, 7:15 hydroseal and 7:16 testicular tumour. 7:20 Investigations to perform include a urine dipstick for blood and infection, low 7:27 threshold for 7:28 urine culture, microscopic culture sensitivity. 7:32 If STI suspected, you want to do a first-word urine for NAD, for gonorrhea, ch 7:38 lamydia and 7:39 often mycoplasma genitalium, plus broader STI screening depending on the 7:44 patient's history. 7:47 Blood such as for blood can and CRP can support infection and consider blood 7:51 cultures if systemically 7:53 unwell. 7:55 Diagnosis is usually clinical, but scrotal doppler ultrasound can be helpful to 7:58 support 7:59 the diagnosis and assess complications such as abscess. 8:04 Doppler may show increased vascularity in Epidinomyitis. 8:08 Importantly, if torsion is strongly suspected, imaging should not delay urgent 8:13 surgical management. 8:21 Most patients with Epidinomyitis can be treated as outpatient, so not inside 8:27 the hospital unless 8:28 they are systemically unwell or have uncontrolled pain or need further 8:34 investigation. 8:36 And for Epidinomyitis include antibiotics, analgesia, rest and scrotal support. 8:44 Antibiotics are usually started empirically based on likely source, so for 8:48 example, enteric 8:49 UTI associated a foroquinolone depending on local guidelines and guidance and 8:57 resistance 8:58 STI associated keftriaxone or plus-minus ductus cyclin with additions based on 9:05 suspected gonorrhea 9:07 and local protocol. 9:10 Advise patients to abstain from sexual activity until treatment is complete and 9:14 symptoms resolve 9:15 and consider partner notification treatment if an STI is confirmed or likely. 9:26 So what about complications? 9:28 Well, symptoms often begin improving within 48 hours of appropriate antibiotics 9:34 . 9:35 Possible complications include reactive hydroseal and rarely abscess formation 9:39 or testicular 9:39 infarctio, which is death of the testis, or part of. 9:44 Persistent or worsening symptoms should prompt reassessment for alternative 9:49 diagnoses, complications 9:51 or resistant organisms. 9:56 for example, the testis is a very important part of the testis.