Overview
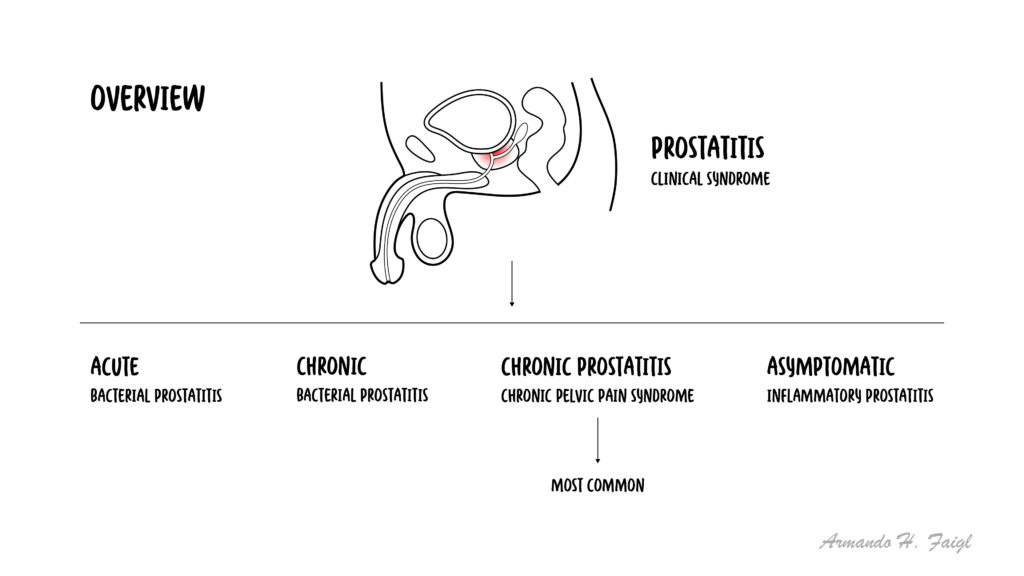
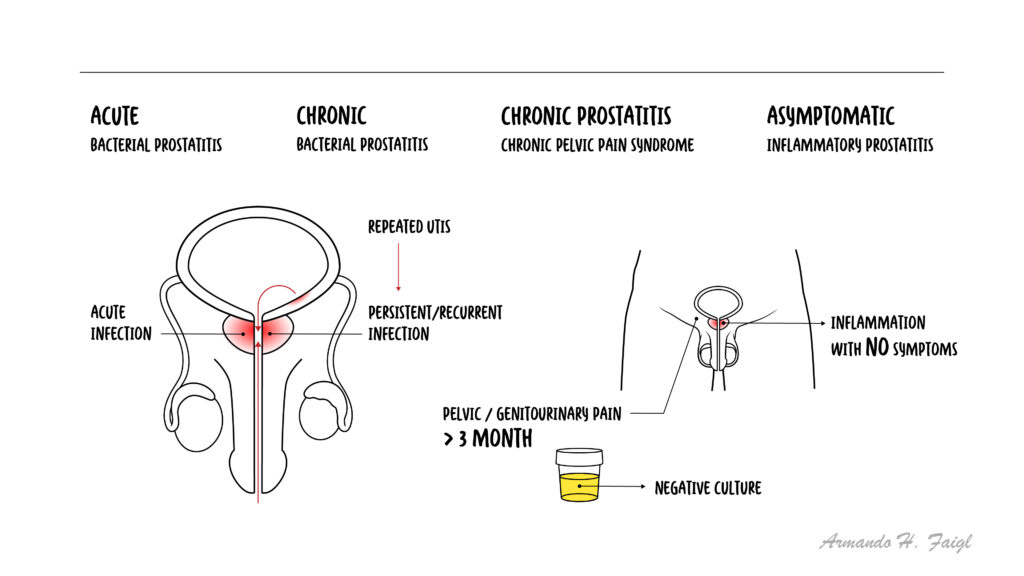
Prostatitis refers to a spectrum of conditions involving inflammation of the prostate gland, ranging from acute bacterial infection to chronic pelvic pain syndromes. It is a common urological condition affecting men of all ages, particularly those aged 30–50 years. The National Institutes of Health (NIH) classifies prostatitis into four categories: acute bacterial, chronic bacterial, chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS), and asymptomatic inflammatory prostatitis. Acute bacterial prostatitis is usually caused by gram-negative organisms such as E. coli, while CP/CPPS is the most common subtype and is often non-infectious.
Definition
Prostatitis: Inflammation of the prostate gland.
Acute bacterial prostatitis: Sudden infection of the prostate with systemic symptoms.
Chronic bacterial prostatitis: Recurrent bacterial infection of the prostate.
Chronic pelvic pain syndrome (CP/CPPS): Chronic pelvic pain without clear infection.
Asymptomatic inflammatory prostatitis: Inflammation without symptoms.
Most prostatitis cases = non-bacterial (CP/CPPS).
Anatomy & Physiology
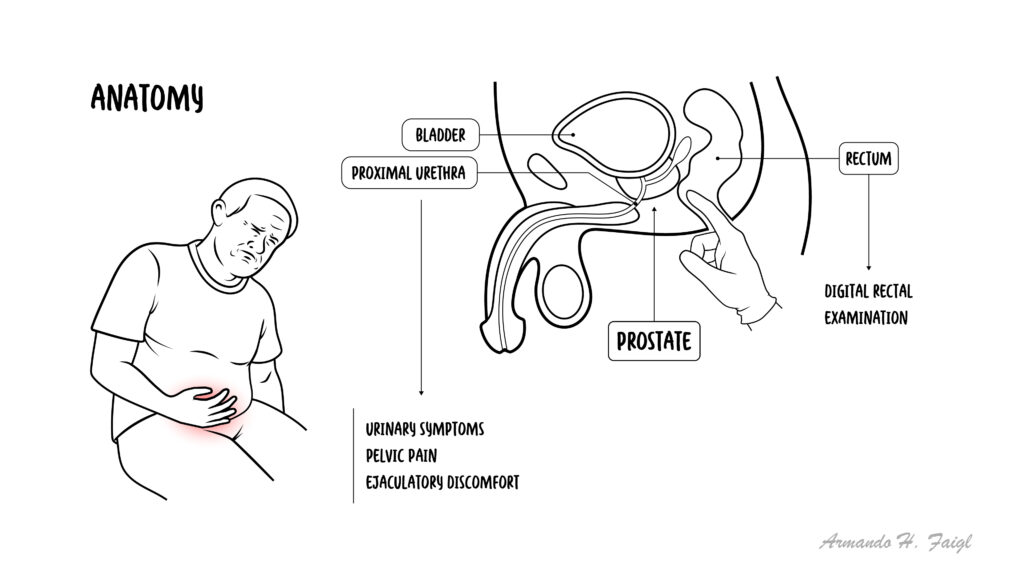
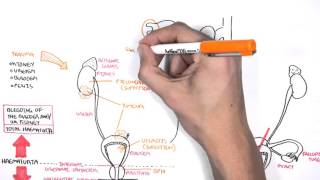
- Prostate gland: Located below bladder, surrounds urethra
- Function: Produces prostatic fluid contributing to semen
- Zones: Peripheral, central, transition zones
- Drainage: Via prostatic ducts into urethra
Aetiology & Risk Factors
- Bacterial infection (E. coli, gram-negative organisms)
- Non-infectious inflammation
- Pelvic floor dysfunction
- Urinary tract infections
- Catheterisation
- Recent urological procedures
- Sexual activity
- Bladder outlet obstruction
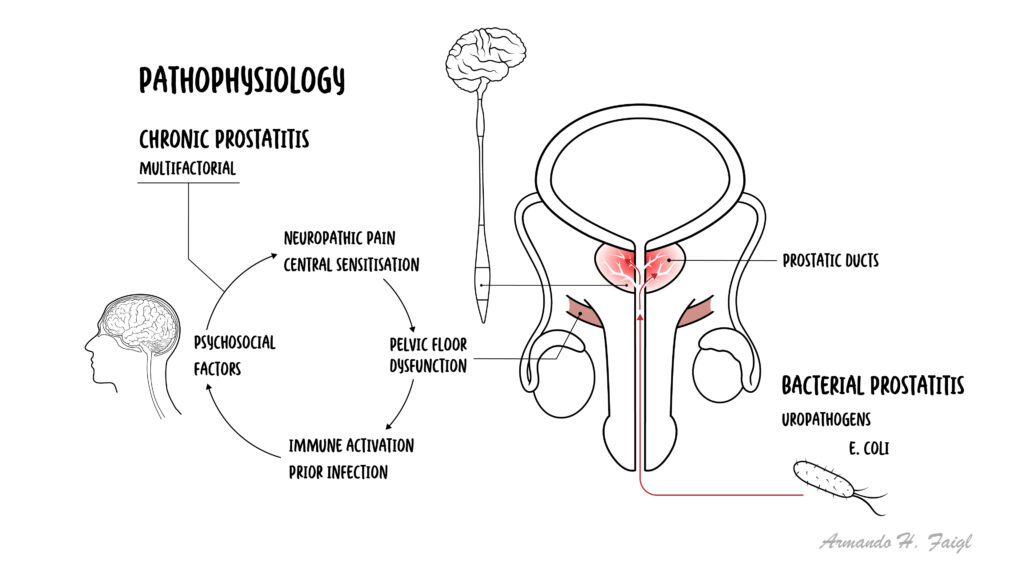
Pathophysiology
Acute bacterial prostatitis
- Ascending infection from urethra or reflux of infected urine into prostatic ducts
- Common organisms: E. coli and other gram-negative bacteria
- Acute inflammation → oedema, glandular swelling → urinary obstruction and pain
- Systemic spread → fever, bacteraemia, sepsis
Chronic bacterial prostatitis
- Persistent bacterial colonisation within prostatic ducts
- Biofilm formation → poor antibiotic penetration
- Recurrent infection → chronic inflammation and fibrosis
Chronic pelvic pain syndrome (CP/CPPS)
- No clear infection
- Neurogenic inflammation → sensitisation of pelvic nerves
- Pelvic floor muscle dysfunction → pain and urinary symptoms
- Psychological factors may contribute (stress, central sensitisation)
Asymptomatic inflammatory prostatitis
- Subclinical inflammation
- Often incidental finding on biopsy or semen analysis
Clinical Manifestations
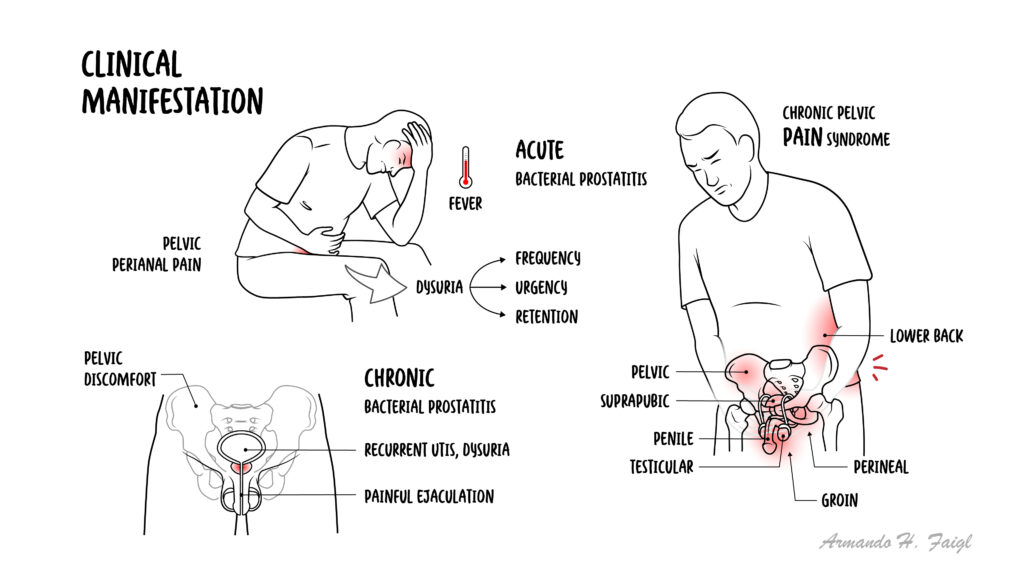
Acute bacterial prostatitis
- Fever, chills, malaise (systemic features)
- Dysuria, frequency, urgency
- Acute urinary retention
- Perineal, suprapubic, or low back pain
- Painful ejaculation
- Tender, boggy prostate on DRE
Chronic bacterial prostatitis
- Recurrent urinary tract infections
- Dysuria, frequency, urgency (milder than acute)
- Perineal or pelvic discomfort
- Pain with ejaculation
- Usually no systemic symptoms
Chronic pelvic pain syndrome (CP/CPPS)
- Chronic pelvic/perineal pain (>3 months)
- Pain with ejaculation
- Urinary symptoms (frequency, urgency, hesitancy)
- Sexual dysfunction
- No identifiable infection
- Exam often normal or mild tenderness
Asymptomatic inflammatory prostatitis
- No symptoms
- Incidental finding on biopsy or semen analysis
Diagnosis
- Urinalysis and culture
- Prostate exam (avoid in acute severe cases)
- PSA (may be elevated)
- Imaging if abscess suspected
Classification
| Type | Description |
| I | Acute bacterial |
| II | Chronic bacterial |
| III | CP/CPPS |
| IV | Asymptomatic |
Treatment
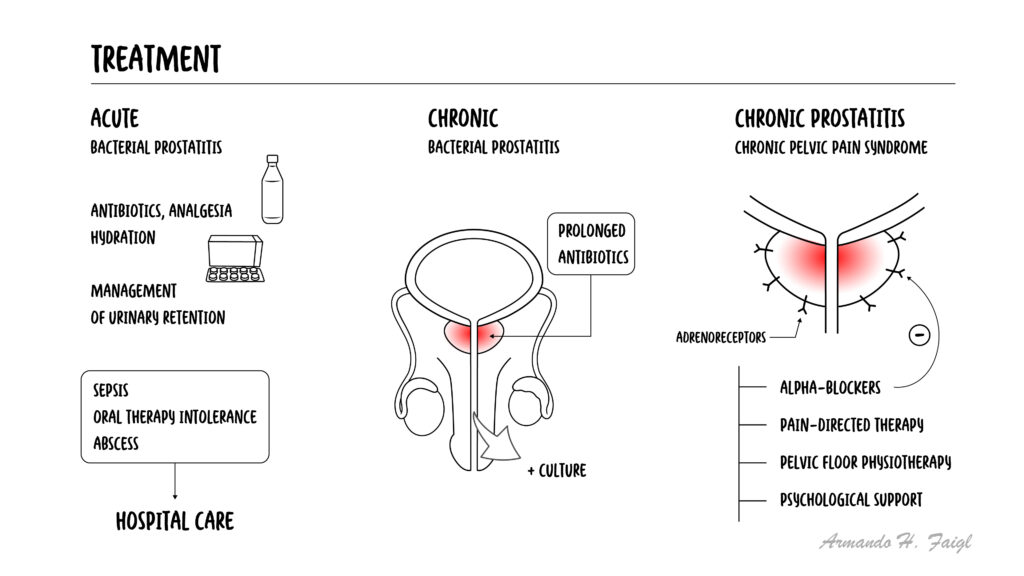
- Acute bacterial: antibiotics (fluoroquinolones, TMP-SMX)
- Chronic bacterial: prolonged antibiotics
- CP/CPPS: alpha-blockers, NSAIDs, pelvic therapy
- Supportive care (hydration, pain control)
Complications and Prognosis
- Prostatic abscess
- Sepsis
- Chronic pelvic pain
- Urinary retention
- Acute: good with treatment
- Chronic: relapsing course
- CP/CPPS: long-term management required
References
- Krieger JN, et al. NIH classification of prostatitis.
- Rees J, et al. Prostatitis guidelines. Eur Urol. 2015.
- NICE Guidelines. Prostatitis.











Discussion