Iron Deficiency Anaemia

In the clinical setting, iron deficiency is the most common cause of anaemia. Iron Deficiency is lack of iron in the body resulting from inadequate iron intake, increased iron loss and increased iron demand which can lead to anaemia. Iron is an integral part of haemoglobin the oxygen carrying protein. Without iron, oxygen is unable to be carried resulting in anaemia.
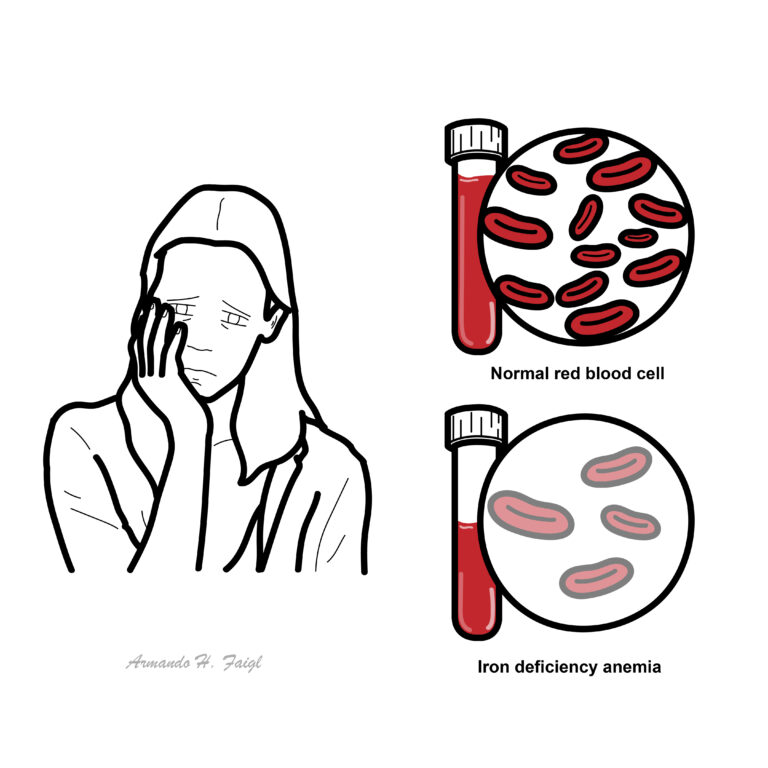
Anaemia (Anemia): The World Health Organization defines anaemia as a haemoglobin (Hb) concentration below 13 g/dl (130 g/L) in men over 15 years of age, below 12 g/dl (120g/L) in non-pregnant women over 15 years of age, and below 11 g/dl (110g/L) in pregnant women
Iron deficiency anaemia: Most common type of anemia, and it occurs when your body doesn’t have enough of the mineral iron
Microcytic anemia Defined as the presence of small, often hypochromic, red blood cells in a peripheral blood smear and is usually characterized by a low mean cell volume (MCV) (<83 micron3). Iron deficiency is the most common cause of microcytic anemia.
Normocytic anaemia: defined by a normal mean corpuscular volume (MCV), but the hemoglobin and hematocrit are decreased. Usually a result of hemolytic anaemia or anaemia of chronic disease
Mactocytic anaemia (Macrocytosis): defined as a mean corpuscular volume greater than 100 fL, is frequently encountered when a complete blood count is performed. The most common etiologies are alcoholism, vitamin B12 and folate deficiencies, and medications.
Epidemiology More than one-quarter of the world’s population is anaemic. Approximately one-half of this burden is a result of iron deficiency anaemia, being most prevalent among preschool children and women. Iron deficiency anaemia occurs in 2–5% of adult men and postmenopausal women in the developed world and is a common cause of referral to gastroenterologists.
Overview Most body iron (ie, 2.6g of 3–4 g) circulates as haemoglobin (Hb), which is recycled when red cells senesce.
Dietary source of Iron
1. Iron is required for the formation of the haem moiety in haemoglobin, myoglobin, and haem enzymes, also known as cytochromes.
2. Iron can also be stored in the form of ferritin
3. Iron Deficiency can be a result of:
4. Anaemia then results in decreased oxygen-carrying capacity and the resultant symptoms of fatigue, low energy level, and dyspnoea on exertion.
Once iron deficiency anaemia is identified, the goal is to determine the underlying aetiology.
Patients with an underlying condition that causes iron deficiency anemia should be treated or referred to a subspecialist (e.g., gynecologist, gastroenterologist) for definitive treatment.
Gastrointestinal, Genitourinary sources of bleeding should always be excluded.
Decrease in iron intake or impaired Absorption
Increase in iron loss
Increase in iron demand
Our body needs iron 1mg/day. Pregnant women need 5-6mg/day.
Anaemia
Iron Deficiency
Patients with iron deficiency anemia are often asymptomatic and have limited findings on examination.
Elder patient presenting with iron deficiency must be investigated for colon cancer malignancy even in the absence of Foecal blood.
Anaemia
Iron Disorder
The lower the haemoglobin the more likely there is to be serious underlying pathology and the more urgent is the need for investigation. Patients without a clear physiological explanation for iron deficiency (especially men and postmenopausal women) should be evaluated by gastroscopy/colonoscopy to exclude a source of gastrointestinal bleeding, particularly a malignant lesion.
In anaemia of chronic disease the RDW decreases the red blood cells are of similar size.
| INTERPRETING PLASMA IRON STUDIES | |||
| Condition | Iron | Total Iron Binding Capacity | Ferritin |
| Iron deficiency | ↓ | ↑ | ↓ |
| Anaemia of chronic disease | ↓ | ↓ | ↑ |
| Chronic Haemolysis | ↑ | ↓ | ↑ |
| Haemochromotosis | ↑ | ↓ (or ↔) | ↑ |
| Pregnancy | ↑ | ↑ | ↔ |
IDA may be effectively diagnosed in most cases by full blood examination and serum ferritin level. Serum iron levels should not be used to diagnose iron deficiency.
A complete blood count can be helpful to determine the mean corpuscular volume or red blood cell size. Although iron deficiency is the most common cause of microcytic anemia, up to 40 percent of patients with iron deficiency anemia will have normocytic erythrocytes.
Diagnosis of iron deficiency anemia requires laboratory-confirmed evidence of anemia, as well as evidence of low iron stores. Anemia is defined as a hemoglobin level two standard deviations below normal for age and sex
Iron deficiency anaemia and thalassaemia trait are the commonest causes of microcytic anaemia, but they may coexist. Serum ferritin and haemoglobin A2 quantitation are the two most important investigations to distinguish between iron deficiency anaemia and thalassaemia trait.
Oral iron therapy, in appropriate doses and for a sufficient duration, is an effective first-line strategy for most patients.
Prognosis
With treatment, the outcome is likely to be good. However, it does depend on the cause (i.e the cause is cancer). Once haemoglobin is corrected, it takes an additional 6 months or so of iron replacement therapy to restore iron stores.
Overview
Worldwide, anemia affects up to one-half of children younger than five years. Anemia is defined as a hemoglobin level that is two standard deviations below the mean for age.
Anemia can be categorized as microcytic, normocytic, or macrocytic. Microcytic iron deficiency anemia is a common cause of childhood anemia, whereas macrocytic anemia is rare in children
Risk Factors
Although iron deficiency anemia is associated with cognitive delays in children, it is unclear if iron supplementation improves cognitive outcomes.
Signs and Symptoms
Other differentials of microcytic anaemia to consider in children
Thalassaemia minor
Alpha Thalassaemia
Rare causes of Microcytic Anaemia
Hypoplastic/Aplastic Anaemia
(eg. acute leukaemia, aplastic anaemia, infiltrative disorders)
UpToDate
Best Practice
Goddard, AF., James, MW., McIntrye, AS., & Scott, BB. 2011. Guidelines for the management of iron deficiency anaemia. Gut. 60. 1309-1316.
Pasricha, SS., Flecknoe-Brown, SC., Allen, KJ., et al. 2010. Diagnosis and management of iron deficiency anaemia: a clinical update. Medical Journal Australia. 193 (9). 525-532.
Short, MW., & Domagalski, JE., 2013. Iron Deficiency Anaemia: Evaluation and Management. American Family Physician. 87 (2). 98-104.

Discussion