Hyperthyroidism (Thyrotoxicosis)
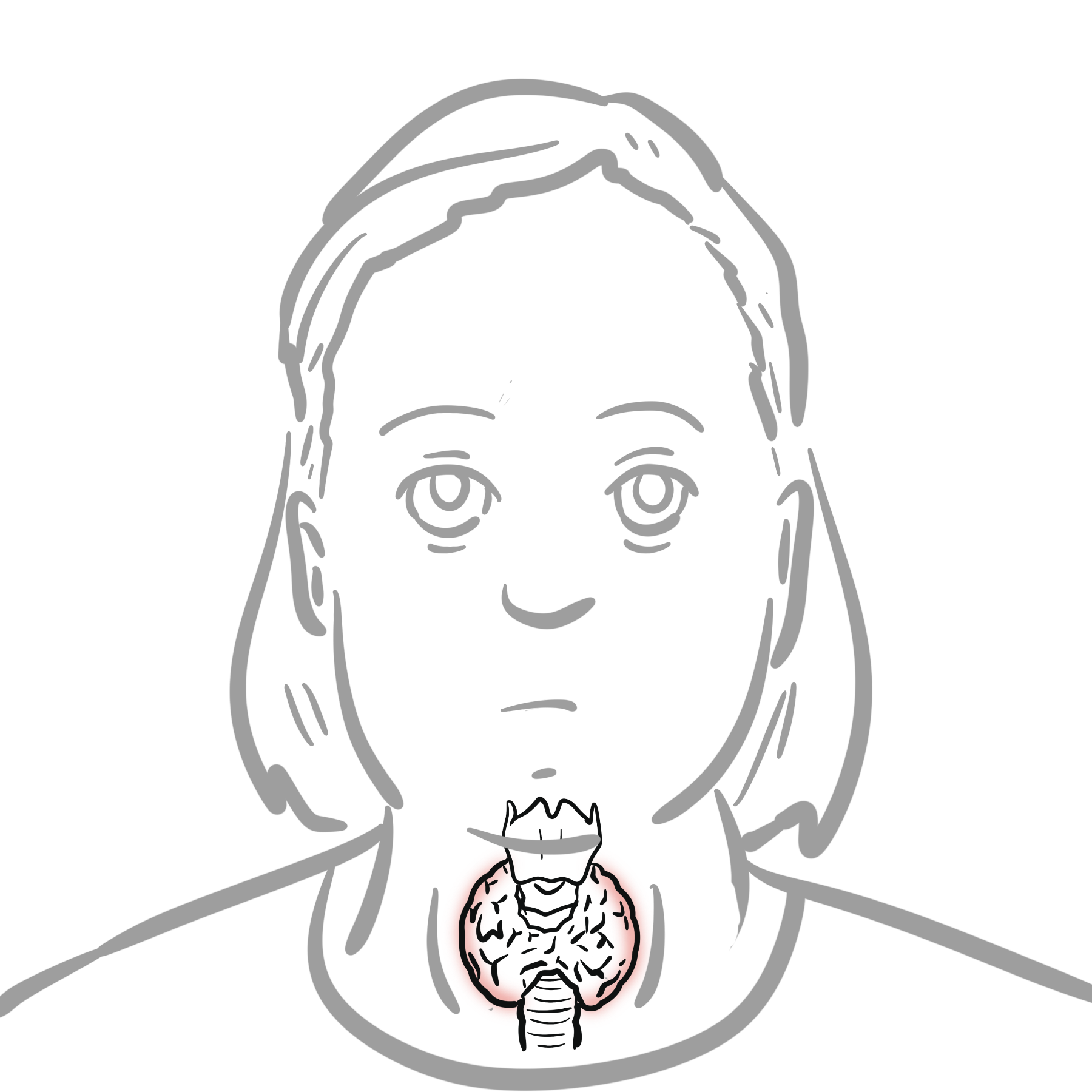

The most common cause of hyperthyroidism are Graves disease, multinodular goitre, an autonomously functioning thyroid nodule (adenoma) and subacute thyroiditis. Graves Disease is more common in women. Multinodular goitre is more common in the elderly. Graves disease typically manifests in middle aged women. Thyroid diseases are more common in women.
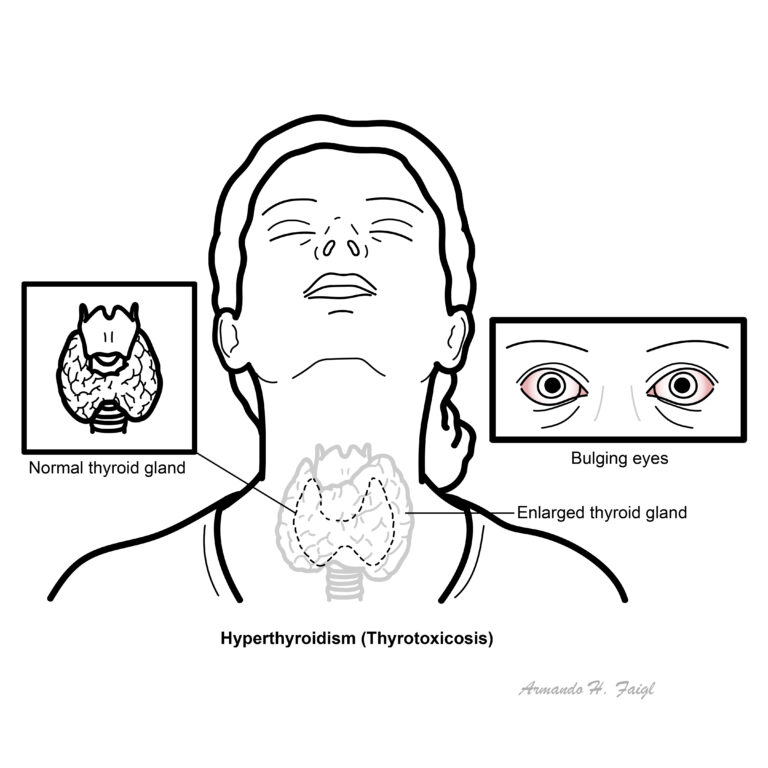
Hyperthyroidism: denote conditions in which hyperfunction of the thyroid leads to thyrotoxicosis.
Hypothyroidism: variety of abnormalities that cause insufficient secretion of thyroid hormones. The most common cause is autoimmune thyroid disease.
Thyrotoxicosis: denotes the clinical, physiological, and biochemical findings that result when the tissues are exposed to excess thyroid hormone. It can arise in a variety of ways (drugs, thyroiditis).
The thyroid gland is butterfly shaped endocrine organ that sits and wraps around the trachea. Anteriorly the thyroid glands are joined by the Isthmus. Developmentally, the thyroid isthmus can give rise to a structure contiguous called the pyramidal lobe, which extends upward.
Posteriorly the thyroid gland does not connect, however 4 parathyroid glands are attached onto the thyroid gland posteriorly.
The gland is in visceral compartment of the neck, along with the trachea, oesophagus and pharynx. The compartment is enclosed in the pre- tracheal fascia, which anchors the thyroid gland to the trachea, so that the thyroid moves up on swallowing.. The thyroid gland stands at the vertebral level C5-T1.
Embryologically, the thyroid gland begins its development at the base of the tongue before descending down to the trachea. This is the reason why thyroid ductal cysts can occur higher up on the neck, anywhere along the path of descent.
Arterial blood supply:
Venous drainage:
Physiology The thyroid gland produces 3 hormones:
1/3 of Amiodarone is Iodine and so can cause hyperthyroidism because iodine is an ingredient for thyroid hormone production.
The main cause of hyperthyroidism is graves disease, an autoimmune disease. In Graves disease, autoantibodies are produced that mimic thyroid stimulating hormone resulting in increase thyroid hormone production leading to hyperthyroidism.
Clinical Examination
| Features of Severe Hyperthyroidism |
| Atrial fibrillation |
| Heart Failure |
| Significant weight loss |
| Proximal myopathy |
Graves Disease Additional Manifestation
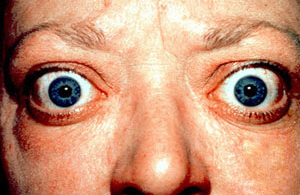
| Conditions associated with Graves Disease |
| Type 1 Diabetes |
| Addison’s Disease |
| Pernicious anaemia |
| Myasthenia Gravis |
| Celiac Disease |
| Vitiligo |
De Quervain’s thyroiditis is acute inflammation of the thyroid gland causing spillage of thyroid hormones into blood stream. Presents with ↑T4,T3, ↑ESR and decreased radioactive iodine uptake.
The clinical presentation of hyperthyroidism is diverse. Neither nuclear thyroid scanning not thyroid ultrasound is a mandatory investigation in hyperthyroidism. If hyperthyroidism has been confirmed by biochemical test (TFT), nuclear thyroid scanning should be considered if the thyroid is no palpable, a single thyroid nodule is detected or thyroiditis is suspected. A normal concentration of TSH rules out a diagnosis of hyperthyroidism.
| Grave’s Disease | De Quervain’s thyroiditis (↑ESR) | |
| TFT’s | Increased | Increased |
| Scintiscanning | Increased | Decreased |
| Management | Antithyroid, B-blocker, radioactive iodine, thyroidectomy | Symptomatic treatment because self resolving – b-blocker, steroids. |
Medical Treatment aim is to induce remission in Graves’ disease, monitor for relapse of treatment and for patients who relapse to consider other treatment options such as radioiodine or surgery.
Thionamides actively accumulates in thyrotoxic tissue and inhibits the action of thyroid peroxidase. Thyroid peroxidase is an enzyme that helps in thyroid hormone synthesis. Agranulocytosis is a life threatening side-effect. Itch and urticarial rash are common side-effects.
Treat patient with antithyroid drug for 18months the aim is remission and prevent relapse. If relapse consider radioiodone or surgery.
Contraindications of radioiodine therapy:Young children, because of the potential risk of thyroid carcinogenesisPregnant and lactating womenSituations where it is clear that the safety of other people cannot be guaranteed.
Surgical treatment Thyroidectomy is rarely recommended for patients with Graves’ disease
| Indications for thyroidectomy |
| Suspicious or malignant thyroid nodule by FNAC |
| Pregnant mothers who are not adequately controlled by ATD |
| Patient reject or fear exposure to radiation |
| Poor compliance to medical treatment |
| Patients who wants rapid control of symptoms |
Complications of thyroidectomy
Thyroid crisis represents a rare but life-threatening exacerbation of the manifestations of thyrotoxicosis.
Clinical signs suggestive of a thyroid storm
Management

Please confirm you want to block this member.
You will no longer be able to:
Please allow a few minutes for this process to complete.
Discussion